Venous Malformations in Children: Early Signs Parents
Published 2026-01-16
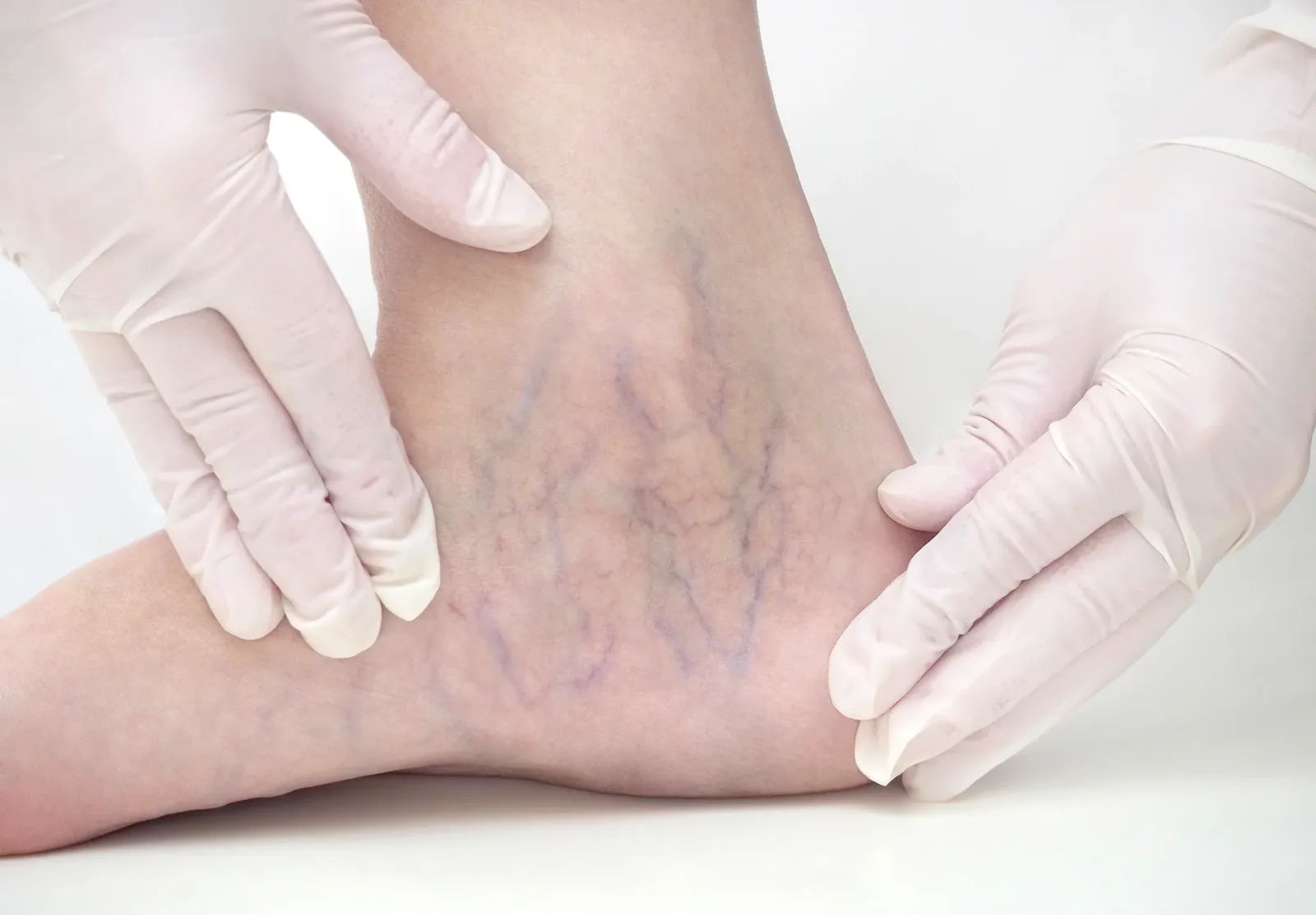
Venous malformations are clusters of veins that did not form normally before birth, creating slow‑flow, low‑pressure vascular channels that can expand over time as a child grows. They are present at birth (congenital) even if they are not always visible in the newborn period and are the most common type of slow‑flow vascular malformation in children.
Unlike “spider veins” or typical bruises, venous malformations are structural anomalies of the venous system and do not simply disappear with time. Because they can enlarge and cause pain, bleeding, or functional problems, early recognition by parents and referral to a specialized vein and vascular anomalies center are critical.
Why Early Detection Matters
A venous malformation can grow proportionally with the child and sometimes expand more rapidly during growth spurts, puberty, or hormonal changes. When left unmonitored, these enlarging malformations can distort nearby skin and soft tissue, limit movement, or create cosmetic differences that affect a child’s confidence.
Early diagnosis also helps prevent complications such as recurrent pain, local clotting within the malformation, or bleeding from fragile surface veins. When pediatric vascular specialists are involved early, treatment options can be planned in stages and timed around key developmental milestones, often with less invasive procedures and better long‑term outcomes.
Early Skin Changes Parents Should Watch For
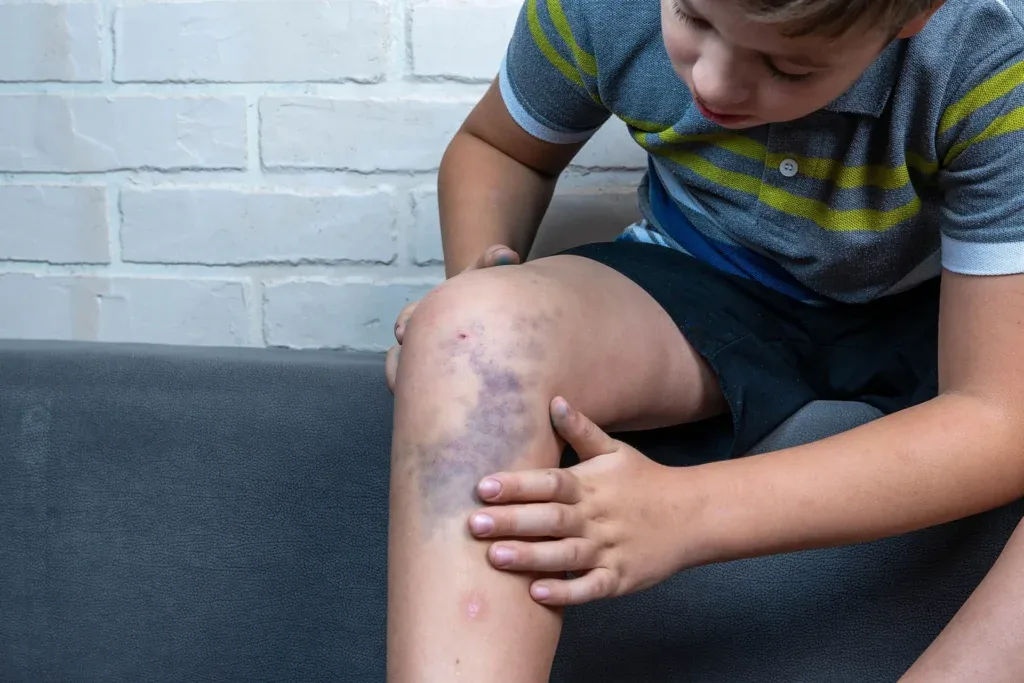
The skin is usually where parents first notice something is different, and pattern‑based observation is one of the strongest “quality signals” for early diagnosis in pediatric vascular disease. Look for:
- One or more maroon, purple, or bluish patches that do not behave like normal bruises and fail to fade on the usual 1–2 week timeline.
- Soft, compressible blue or purple “spongy” areas under the skin that refill when you release gentle pressure or when the child stands up.
- A bulge or swelling with normal overlying skin color that still feels different from the surrounding tissue, especially if it has a rubbery or “bag of worms” texture.
- A bluish patch that darkens or enlarges when the child cries, strains, exercises, or when the area hangs below heart level (for example, a foot lesion when standing).
These cutaneous signals are the surface expression of an underlying venous network; documenting what they look like at baseline and how they change with position or activity gives Vein Center Doctor's team valuable diagnostic context.
Swelling, Pain, and Tenderness
Venous malformations are low‑flow, but blood can pool inside them, leading to chronic congestion and intermittent pain. Parents should be attentive to:
- Recurrent swelling in the same limb, face, or body area, especially when it worsens in the evening, after long periods of standing, or after sports.
- Complaints of dull, aching pain, heaviness, or fullness in a specific spot that correspond to a visible discoloration or lump.
- Tender nodules or cords within a known malformation that feel firmer than usual, which can indicate local thrombosis (clotting) inside the abnormal veins.
Children may not always verbalize pain clearly, so behavior changes: avoiding use of a limb, limping, or refusing certain activities, can be as informative as verbal complaints.
Functional Changes: Movement, Breathing, and Daily Activities
As a venous malformation enlarges or extends deeper, it can begin to interfere with how a child moves, speaks, eats, or breathes. Parents should monitor for:
- Reduced range of motion or stiffness in a joint near a visible malformation, such as difficulty fully bending a knee or elbow.
- Limping, toe‑walking, or altered gait when the malformation involves the foot, ankle, or leg.
- Snoring, noisy breathing, or swallowing difficulties in children with lesions in the tongue, cheek, jaw, or neck.
Early functional limitations are “outer‑section” signs of a deeper vascular problem: they may seem subtle but, when documented and connected to the visible skin findings, they strengthen the diagnostic “information graph” your child’s clinicians build over time.
Bleeding, Bruising, and Clotting Red Flags
While many venous malformations remain stable for years, some develop fragile surface veins or internal clotting that signal higher risk. Seek prompt evaluation if you notice:
- Recurrent bleeding from a patch or nodule on the skin, inside the mouth, or in the nose that is hard to control with simple pressure.
- Rapidly appearing bruises over or around a known malformation without appropriate trauma history.
- Sudden, intense pain and firm swelling inside the lesion, which may represent a thrombosed (clotted) venous lake requiring specialist input.
Because some venous malformations are associated with mild coagulation abnormalities, comprehensive evaluation in a dedicated center helps determine whether additional bloodwork or imaging is needed.
Venous Malformations vs Other Vascular Birthmarks
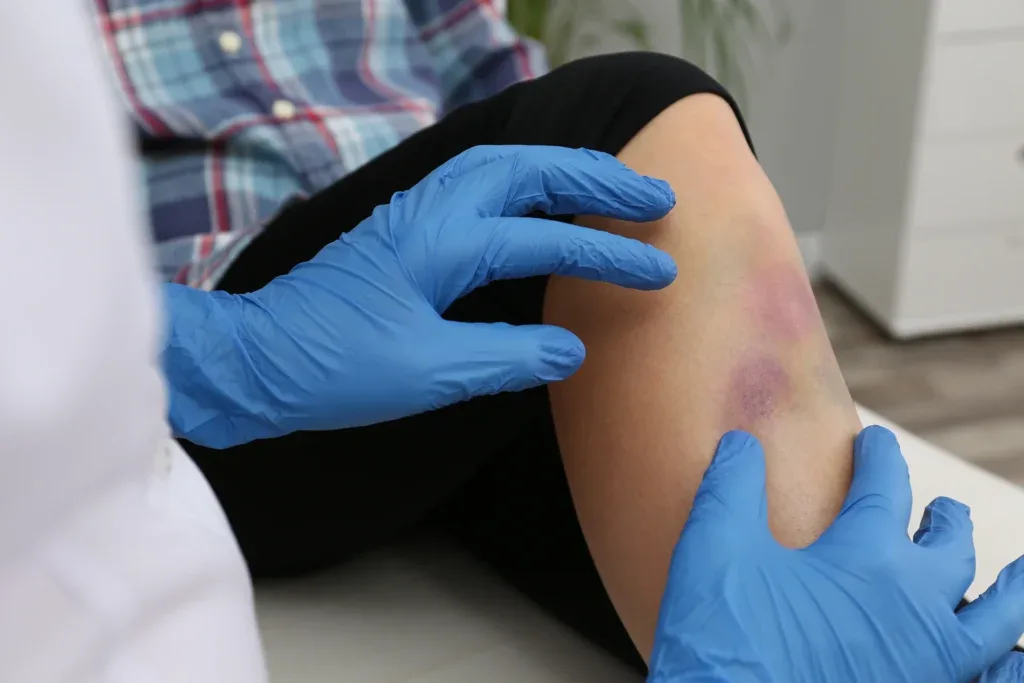
Parents often confuse venous malformations with “birthmarks” such as port‑wine stains or infantile hemangiomas, but these entities behave differently and require different follow‑up.
Key Differences Parents Should Know
Feature
Venous malformation (VM)
Infantile hemangioma
Capillary/port‑wine stain
Present at birth
Yes, but may be subtle
Often appear in first weeks of life
Yes, flat red‑purple patch
Color
Blue, purple, or normal skin over a soft mass
Bright red or deep red “strawberry” phase
Pink to deep purple, flat
Growth pattern
Grows with child, may enlarge in spurts
Rapid growth then slow involution
Enlarges proportionally, may darken
Texture
Soft, compressible, spongy
Raised, rubbery during growth phase
Flat, not compressible
Behavior with gravity/strain
Darkens or bulges when dependent or with crying
Less influenced by position
Usually unchanged with gravity
Understanding where your child’s lesion fits in this table helps you and Vein Center Doctor's team navigate the right diagnostic and treatment pathway rather than following a generic “birthmark” label.
When to Call a Specialist vs the Pediatrician
Primary care pediatricians are an essential first touchpoint, but venous malformations sit in a highly specialized niche that overlaps dermatology, interventional radiology, and vascular surgery. Early co‑management with a dedicated vein and vascular anomalies center increases the “authority” and precision of your child’s care pathway.
Consider contacting a specialist center like Vein Center Doctor at Vein Center Doctor if:
- The discoloration or swelling has been present for more than 4–6 weeks without fading or explanation.
- The lesion is enlarging, becoming more painful, or affecting movement, vision, breathing, or feeding.
- There is recurrent bleeding, frequent new bruising over the same area, or sudden firm, painful changes.
For very small, stable lesions without symptoms, your pediatrician and the specialist team may choose careful observation with periodic imaging, but that decision should follow at least one expert evaluation rather than assumption.
How Vein Center Doctor and Vein Center Doctor Evaluate These Lesions

Vein Center Doctor's approach aligns with an “engineering‑minded” vascular strategy: define the entity precisely, map its attributes, and then design targeted interventions. Evaluation typically involves:
- A detailed history focusing on onset, triggers, growth pattern, pain cycles, bleeding episodes, and functional impact.
- High‑resolution physical examination, often with positional maneuvers (standing vs lying, strain vs rest) to assess compressibility and flow behavior.
- Non‑invasive imaging such as Doppler ultrasound and, where indicated, MRI to define depth, extent, and relation to muscles, joints, or vital structures.
This structured evaluation builds an internal “information graph” of your child’s malformation, connecting clinical signs, imaging attributes, and risk factors, so treatment decisions remain consistent and transparent over time.
Treatment Options and Long‑Term Outlook
Many venous malformations can be managed effectively with a staged, child‑centered plan, and not every lesion requires immediate intervention. For symptomatic or high‑risk malformations, Vein Center Doctor and similar centers may employ:
- Image‑guided sclerotherapy, in which a specialist injects a solution directly into the abnormal veins to shrink or shut them down over multiple sessions.
- Surgical excision, often after sclerotherapy has reduced the size and bleeding risk of the lesion, particularly when it causes functional limitation or significant disfigurement.
- Supportive measures such as compression garments for limb lesions, pain management protocols, and physical therapy to protect joint function.
With appropriate follow‑up, many children go on to lead active, unrestricted lives, and early, precise treatment can minimize long‑term cosmetic and functional impacts.
Practical Checklist for Parents
To reduce the “cost of retrieval” for parents in daily life, it helps to translate the above signals into a simple, repeatable checklist.
Ask yourself once a month:
- Is there any patch or lump on my child’s skin that is blue, purple, or maroon and has not faded the way a normal bruise would?
- Does any visible spot grow darker, puffier, or more painful when my child cries, stands for long periods, or plays sports?
- Has my child started to limp, avoid using a limb, or complain of heaviness or aching in one specific area?
- Have I seen bleeding, frequent bruising, or sudden, firm swelling in a known lesion?
- Is the lesion near a critical area—eye, airway, mouth, joints, or genital region—where small changes could have big effects?
If you answer “yes” to any of these questions, capturing clear photos and scheduling an evaluation with a pediatric‑experienced vein specialist like Vein Center Doctor at Vein Center Doctor is the next logical step. Early pattern recognition from parents, coupled with expert mapping and treatment, offers children the best chance for healthy growth with minimal interruption from their venous malformations.