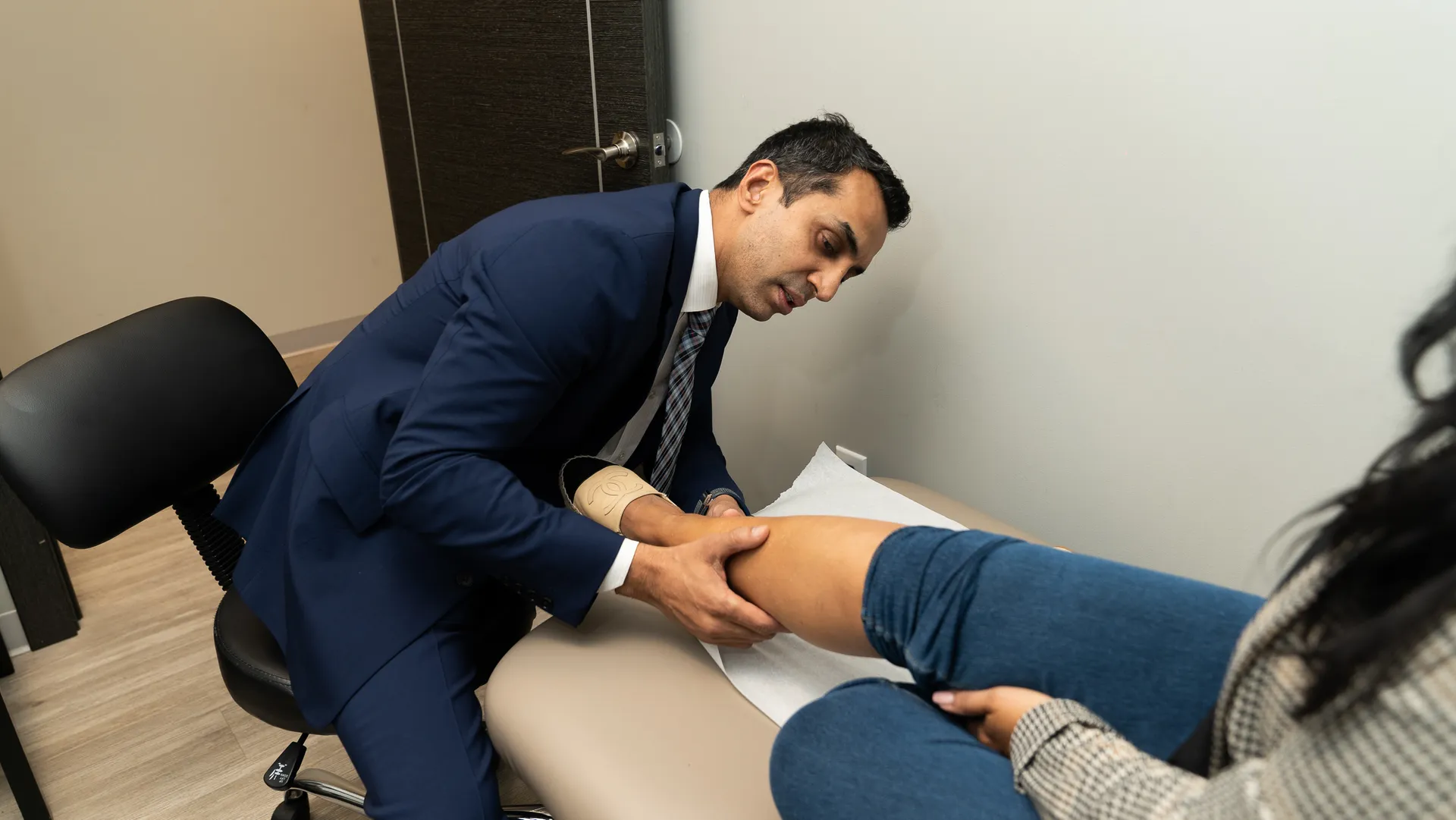
Pelvic Congestion Syndrome: The Overlooked Vein Disease in
Published 2025-11-26

Pelvic Congestion Syndrome is an overlooked vein disease causing chronic pelvic pain in women due to varicose veins in the pelvis from venous insufficiency, which is definitively treated with minimally invasive pelvic vein embolization.
What Is Pelvic Congestion Syndrome?
Pelvic Congestion Syndrome (PCS) is a chronic vascular condition affecting women that causes persistent pelvic pain due to varicose veins developing in the pelvic region, particularly within the ovarian and pelvic veins that become dilated, tortuous, and congested from venous insufficiency or obstruction. Unlike visible varicose veins in the legs, pelvic varicosities remain hidden deep within the pelvis, making PCS one of the most underdiagnosed causes of chronic pelvic pain, affecting an estimated 30% of women experiencing chronic pelvic discomfort.
Despite its prevalence, many women suffer for years without proper diagnosis because the symptoms mimic other gynecological conditions such as endometriosis, ovarian cysts, or irritable bowel syndrome. The condition typically affects women of childbearing age who have had multiple pregnancies, though it can occur in women who have never been pregnant.
Understanding PCS as a vein disease, not just a "women's issue", represents a critical shift in how we approach chronic pelvic pain and opens pathways to effective, minimally invasive treatments.
The Hidden Symptoms Women Often Dismiss

Chronic Pelvic Pain: The Primary Indicator
The hallmark symptom of Pelvic Congestion Syndrome is a persistent dull, aching, or "dragging" pain in the pelvis or lower abdomen that lasts for more than six months and worsens throughout the day, particularly after prolonged standing or sitting. This pain differs from acute conditions because it follows a predictable pattern: mild discomfort in the morning that intensifies as gravity pulls blood into the already weakened pelvic veins by afternoon and evening.
Women often describe the sensation as pressure, heaviness, or fullness in the lower abdomen and pelvic region. The pain typically worsens during menstrual periods, after sexual intercourse (dyspareunia), and with any activity that increases abdominal pressure such as lifting, exercise, or even coughing.
Lower Back and Leg Pain
Studies indicate that approximately 50% of women with Pelvic Congestion Syndrome develop pain in their lower back and flank areas, which many patients and even physicians mistakenly attribute to musculoskeletal issues rather than vascular dysfunction. This referred pain occurs because the congested pelvic veins share nerve pathways with the lower back region.
Additionally, patients may experience leg pain, achiness, and swelling in the lower extremities, especially after prolonged periods of standing or sitting. These symptoms often improve when lying down or elevating the legs, which reduces venous pressure in the pelvic region.
Unexpected Varicose Veins
Up to 55% of women with Pelvic Congestion Syndrome develop visible varicose veins in unexpected locations: the upper inner thighs, back of the thighs, buttocks, vulva, and vaginal area. These vulvar varicosities represent one of the most specific clinical signs of PCS, yet many women feel embarrassed to mention them or assume they're normal after pregnancy.
The appearance of varicose veins in these areas indicates that the incompetent pelvic veins are creating backflow and pressure that extends to the superficial venous system.
Urinary and Digestive Symptoms
Pelvic Congestion Syndrome can cause an irritable bladder with symptoms of urinary frequency, urgency, and even stress incontinence due to the pressure exerted by engorged pelvic veins on the bladder. Many women find themselves needing to urinate frequently throughout the day without a urinary tract infection.
Similarly, PCS can trigger irritable bowel symptoms including recurrent abdominal pain, bloating, and alternating episodes of diarrhea and constipation. The congested veins surrounding the intestines interfere with normal digestive function and contribute to abdominal discomfort.
Menstrual Irregularities
Women with Pelvic Congestion Syndrome frequently experience severe menstrual cramps (dysmenorrhea) and heavy menstrual bleeding (menorrhagia) that worsen their already chronic pelvic pain. The hormonal fluctuations during the menstrual cycle cause additional dilation of the already incompetent pelvic veins, intensifying pain and discomfort.
Understanding the Root Causes
Venous Insufficiency and Valve Dysfunction
The exact etiology of Pelvic Congestion Syndrome involves multiple factors, but the primary mechanism is venous insufficiency caused by weakened or absent valves in the ovarian and pelvic veins. Normally, one-way valves in veins prevent blood from flowing backward, but when these valves fail, blood pools in the pelvic region creating varicosities.
The left ovarian vein is particularly susceptible because it drains into the left renal vein at a perpendicular angle, creating higher pressure compared to the right ovarian vein which drains directly into the inferior vena cava. This anatomical difference explains why symptoms often present more prominently on the left side.
Hormonal Influences
Hormones, particularly estrogen and progesterone, play a significant role in the development and progression of Pelvic Congestion Syndrome. Estrogen causes vein walls to relax and dilate, which explains why PCS predominantly affects women of reproductive age and why symptoms often worsen during pregnancy and menstruation when estrogen levels fluctuate.
Multiple pregnancies increase the risk of developing PCS because pregnancy dramatically increases pelvic blood volume while simultaneously causing vein walls to relax, creating conditions favorable for venous insufficiency and valve incompetence.
Venous Obstruction
In some cases, Pelvic Congestion Syndrome results from mechanical obstruction of pelvic veins rather than valve failure alone. Conditions such as May-Thurner syndrome (compression of the left iliac vein by the right iliac artery) or Nutcracker syndrome (compression of the left renal vein) can impede normal venous drainage and contribute to pelvic venous congestion.
Secondary Medical Conditions
Pelvic Congestion Syndrome can occur secondary to other medical conditions including peripheral artery disease, which affects overall vascular function and venous return. The stasis of blood in dilated veins triggers the release of pain-inducing inflammatory substances, which explains the chronic aching pain characteristic of PCS.
How Pelvic Congestion Syndrome Is Diagnosed
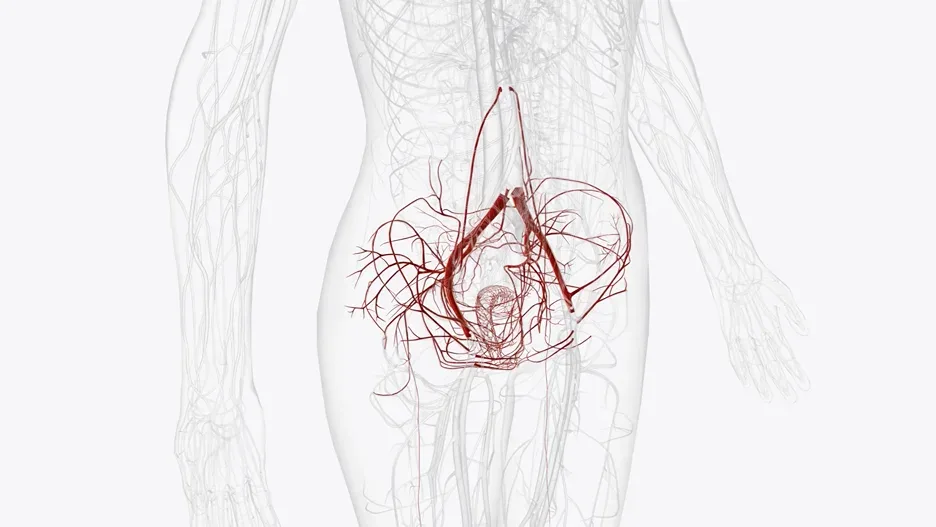
Clinical Evaluation and Physical Examination
Diagnosis begins with a comprehensive clinical history focusing on the pattern of pelvic pain: specifically whether it worsens with standing, during menstruation, and after intercourse. The presence of chronic pelvic pain lasting more than six months combined with ovarian point tenderness on physical examination is 94% sensitive and 77% specific for Pelvic Congestion Syndrome.
However, clinical symptoms alone cannot definitively confirm PCS because many other conditions present with similar pain patterns. Advanced imaging is essential to visualize the pelvic varicosities and confirm venous insufficiency.
Doppler Ultrasound
Transvaginal or transabdominal Doppler ultrasound serves as the first-line imaging modality for diagnosing Pelvic Congestion Syndrome due to its non-invasive nature and ability to assess blood flow dynamics. Diagnostic criteria include ovarian vein diameter of 6 mm or greater (some studies suggest 7 mm as the cutoff), slow blood flow velocity less than 3 cm/s, and retrograde venous blood flow in the ovarian veins.
Ultrasound has a positive predictive value of 83.3% for diagnosing PCS when the ovarian vein diameter reaches 6 mm, making it a reliable screening tool. However, it's important to note that dilated ovarian veins with incompetent valves can be found in asymptomatic women, so imaging findings must always be correlated with clinical symptoms.
CT and MRI Imaging
Computed tomography (CT) and magnetic resonance imaging (MRI) provide detailed cross-sectional images of the pelvic vasculature and can identify dilated, tortuous ovarian and pelvic veins that characterize Pelvic Congestion Syndrome. These modalities are particularly useful when ultrasound findings are equivocal or when comprehensive evaluation of pelvic anatomy is needed.
MRI offers the advantage of excellent soft tissue contrast without radiation exposure, making it ideal for younger women of childbearing age.
Pelvic Venography: The Gold Standard
Ovarian and iliac catheter venography remains the gold standard for definitively diagnosing Pelvic Congestion Syndrome. This minimally invasive procedure involves threading a catheter through the venous system (typically from the groin or neck) into the ovarian veins while using X-ray guidance.
Contrast dye is injected to visualize the veins, and diagnostic criteria include incompetent pelvic veins with diameter greater than 5-10 mm, congestion and slow flow in the ovarian, pelvic, vulvovaginal, and thigh veins, and demonstration of venous reflux during Valsalva maneuver. Venography can be performed under local anesthesia and may transition directly into treatment via embolization during the same session.
Treatment Options That Work
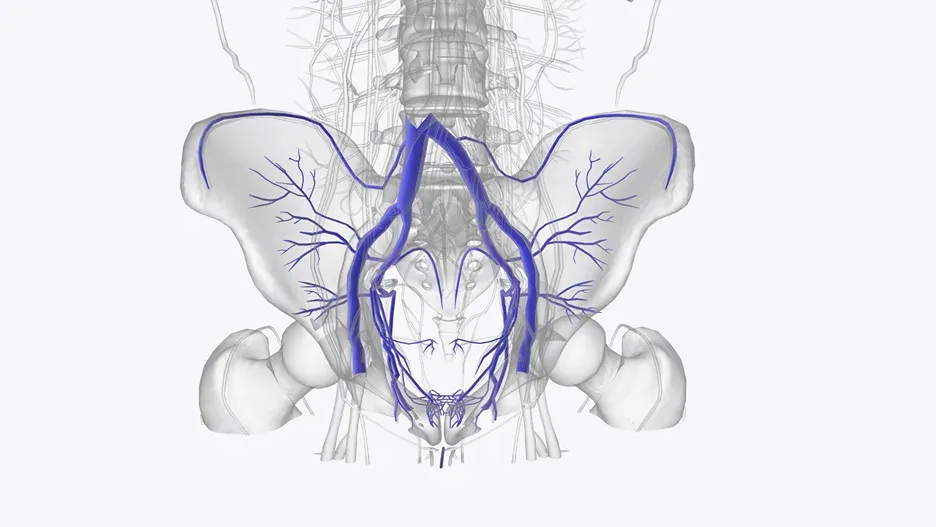
Medical Management: First-Line Approach
Medical management represents the first-line treatment for Pelvic Congestion Syndrome due to its non-invasive nature and lower risk profile. Pharmacological options include gonadotropin-releasing hormone (GnRH) agonists such as goserelin, which suppress ovarian function and reduce estrogen-mediated vein dilation.
Progestins including medroxyprogesterone acetate and etonogestrel implants have demonstrated success in alleviating PCS pain by counteracting estrogen's effects on vein walls. Combined oral contraceptives, danazol, and phlebotonics (medications that improve venous tone) also provide symptom relief for some women.
Nonsteroidal anti-inflammatory drugs (NSAIDs) help manage the chronic inflammatory pain associated with venous congestion. While medical therapy can control symptoms, it does not address the underlying venous insufficiency and typically requires ongoing medication use.
Pelvic Vein Embolization: The Definitive Solution
For women who do not respond adequately to medical therapy, transcatheter pelvic vein embolization has emerged as the preferred definitive treatment for Pelvic Congestion Syndrome. This minimally invasive, non-surgical procedure has proven to be safe, effective, and durable with high success rates.
During embolization, a vascular specialist threads a catheter into the incompetent ovarian and pelvic veins using the same approach as diagnostic venography. Small coils, sclerosing agents, or embolic plugs are then deployed to deliberately block the dysfunctional veins, redirecting blood flow to healthy veins with competent valves.
The procedure is typically performed under local anesthesia with conscious sedation, requires no incisions, and allows patients to return home the same day. Most women experience significant pain relief within the first few weeks as the congested veins shrink and venous pressure normalizes.
Embolization offers superior outcomes compared to medical management alone and avoids the risks and recovery time associated with surgical approaches. The procedure can target both the ovarian veins and internal iliac veins depending on the pattern of venous insufficiency identified during venography.
Surgical Options
Surgical treatments for Pelvic Congestion Syndrome include ovarian vein ligation (tying off the incompetent veins), hysterectomy with bilateral oophorectomy (removal of uterus and ovaries), and laparoscopic vein resection. However, clinical practice has increasingly shifted away from surgical approaches toward percutaneous embolization as the definitive management for PCS due to embolization's lower morbidity and comparable or superior effectiveness.
Surgery may be considered in select cases where embolization is not feasible or when concurrent gynecological conditions require surgical intervention.
Why Pelvic Congestion Syndrome Remains Overlooked
The Diagnosis Gap
Despite affecting millions of women, Pelvic Congestion Syndrome remains significantly underdiagnosed because its symptoms overlap with numerous other conditions and because the varicosities are not externally visible like leg varicose veins. Many women endure years of chronic pain while undergoing extensive gynecological workups that fail to identify the vascular etiology.
The condition is analogous to varicocele in men (dilated testicular veins causing pain and fertility issues), but unlike varicoceles which are easily detected through physical examination, pelvic varicosities in women require specialized imaging to visualize.
Lack of Awareness Among Healthcare Providers
Many primary care physicians and even gynecologists have limited familiarity with Pelvic Congestion Syndrome as a distinct clinical entity, often attributing chronic pelvic pain to musculoskeletal issues, endometriosis, or psychosomatic causes. This knowledge gap delays diagnosis and proper referral to vascular specialists who can provide definitive treatment.
The Stigma of "Invisible" Pain
Women with chronic pelvic pain frequently face dismissal of their symptoms, being told their pain is "normal" or "all in their head". Because Pelvic Congestion Syndrome produces no external signs except occasional vulvar varicosities that women may feel embarrassed to mention, the condition remains hidden and untreated.
When to Seek Vascular Evaluation
Women should seek evaluation by a vein specialist if they experience chronic pelvic pain lasting more than six months that worsens with standing, during menstruation, or after sexual intercourse, especially if accompanied by visible varicose veins in the vulva, thighs, or buttocks. Additional red flags include lower back pain that improves with lying down, urinary frequency without infection, and abdominal bloating that varies throughout the day.
Early diagnosis and treatment of Pelvic Congestion Syndrome can dramatically improve quality of life by eliminating chronic pain, reducing reliance on pain medications, and addressing the underlying vascular dysfunction. At The Vein Center, board-certified vascular specialists led by Dr. Rahul Sood offers comprehensive evaluation and advanced treatment options including pelvic vein embolization in a Joint Commission Accredited facility.
Ready to find relief from chronic pelvic pain? Book your consultation with The Vein Center today. Dr. Sood and our expert team specialize in diagnosing and treating Pelvic Congestion Syndrome using the latest minimally invasive techniques. Most insurances accepted.