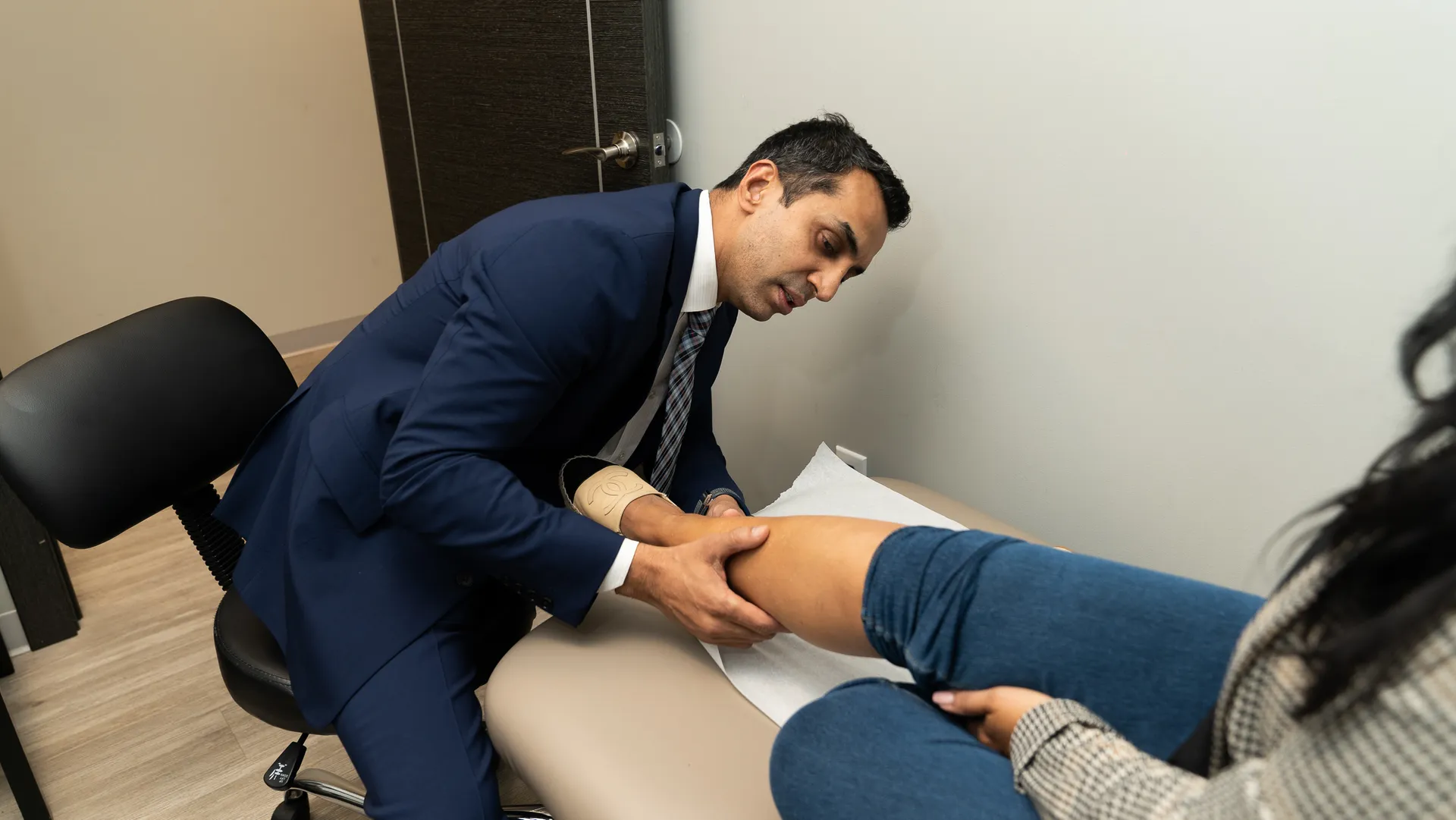
Can Varicose Veins Cause Blood Clots?
Published 2021-09-03
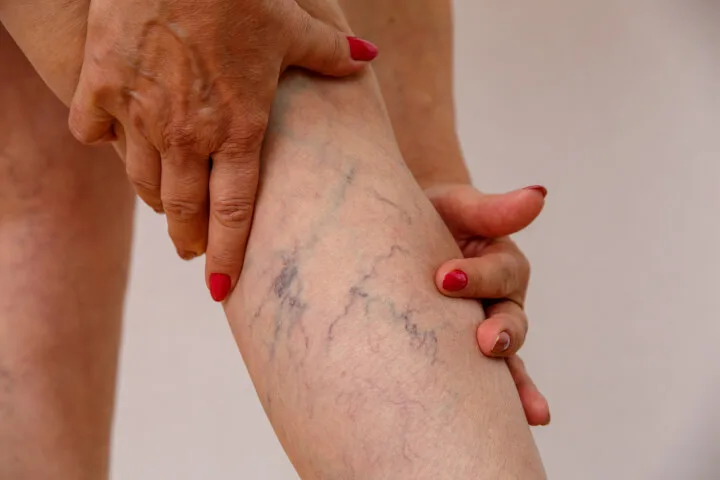
Having varicose veins is more common than you think. Nearly a quarter of adults have these large, twisted cords on the legs and many of them are trying out ways to cover the unsightly veins or seek treatment options to eliminate them completely. But apart from its unappealing appearance, varicose veins can also lead to more serious health concerns, such as blood clots.
So how can varicose veins cause blood clots and what can you do about it? Although it’s possible to develop blood clots due to varicose veins, it’s a comparatively rare occurrence. Most varicose veins are located just below the surface of the skin and most blood clots form there too. Most people never get the condition though. Still, it helps to know the causes and what you can do just in case.
Risk Factors for Varicose Veins
There are several factors that contribute to a person developing varicose veins, but the most prevalent are genetics and increased pressure in veins. Women, due to their hormonal imbalances, are more at risk of getting these veins than men, especially if you count those who are taking contraceptive pills, pregnant women, and menopausal women. Obesity, aging, injuries, smoking, and an unhealthy lifestyle can also greatly increase your chances of getting varicose veins.
Varicose veins symptoms may vary from person to person, but the most common ones are skin discoloration, sores on the legs, rashes, and sensations in the legs, such as aching, burning, or a heavy feeling.
Learn More: When To Worry About Varicose Veins?
How Varicose Veins Turn Into Blood Clots
There’s a long journey involved in the upward flow of blood from the feet to the heart, and forces of gravity make the flow even more challenging. This can result in the venous structure breaking down eventually, which leads to the discoloration, swelling, and twisting of veins.
When the valves fail to regulate blood flow, the blood can begin to collect and settle. Such pooling can lead to the formation of blood clots, which further impedes the regular flowing of blood. Not only can these blood clots become painful, but they can also lead to further health complications that should be addressed by the doctor immediately.
Difference Between a Blood Clot in a Superficial Vein and Deep Leg Vein
Superficial blood clots are referred to as superficial thrombophlebitis, phlebitis, or superficial venous thrombosis. This usually occurs due to injury, which can cause sudden inflammation in the vein and cause blood flow to slow down and blood clots to form. Superficial veins aren’t surrounded by muscle, unlike deeper blood vessels. Muscles function as pumps for your veins. If there’s no pump to move it out, blood clots could stick to the vein wall and become difficult to dislodge.
This is why your varicose veins feel like a hard cord and become painful. Fortunately, the problem usually goes away on its own, and inflammation decreases after a few days. The hardness of the vein subsides after a few weeks. You can ease your pain and other symptoms by applying a warm compress and taking aspirin.
These clots in the varicose vein can cause swelling, redness, pain, and tenderness in the leg or around the affected vein itself, but they don’t usually reach the lungs or lead to a pulmonary embolism (PE) or blood clot in the lung.
Deep vein thrombosis or DVT, on the other hand, is a serious condition and doesn’t usually happen within the varicose veins, except for severe cases. A study that was published in the Journal of the American Medical Association shows that people with varicose veins are five times more likely to have deep venous thrombosis.
It’s similar to superficial thrombophlebitis, but the deep vein blood clots form in the larger, deeper veins, which are bigger vessels that carry more blood to other parts of the body.
If these clots get squeezed out of your leg by your muscles, they could go elsewhere in your body and do a lot of damage. And when it settles in your lungs, it can cause pulmonary embolism, which is a life-threatening condition.
It can be difficult to tell the difference between blood clotting in a superficial vein and one in a deep leg vein, which is why it's best to consult with a vein specialist. Only he can spot superficial thrombophlebitis and venous thromboembolism on appearance alone.
It's tricky to diagnose DVT since some people experience no symptoms and if there are, it can be similar to superficial thrombophlebitis. Signs of a potential DVT include swelling, tenderness, skin that’s red, warm, and discolored, pain in the calf, foot, and leg, and sudden leg fatigue.
Since the difference between the two conditions is subtle, a visit to the doctor is necessary for an accurate diagnosis. You never know if you’ll need vein surgery for your painful varicose veins as a result of a complication such as a clot formation.
If it’s just superficial thrombophlebitis, you can manage your leg swelling and leg pain problem with home remedies such as wearing compression stockings. Your doctor can also recommend lighter vein problem procedures to fix superficial clots such as sclerotherapy. If it’s DVT, your vein specialist or vascular surgeon will recommend the best kind of treatment for your severe varicose vein.
Learn More: What Are The Options For Varicose Vein Surgery?
Know the State of Your Varicose Veins When You Visit Vein Center Doctor
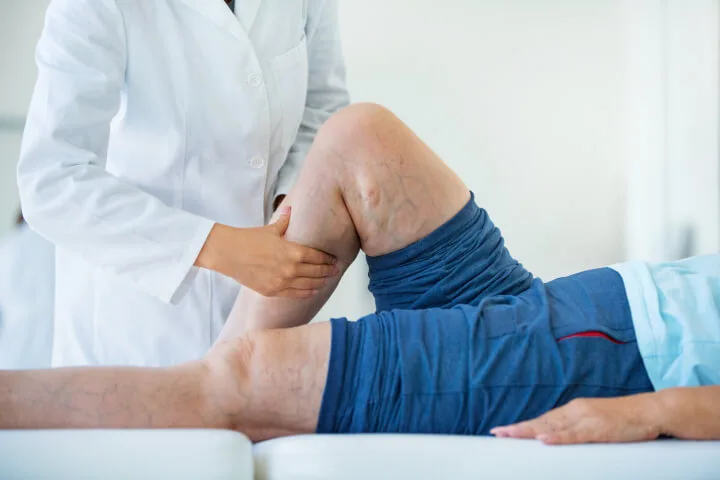
You don't have to let your untreated varicose veins cause complications. Vein Center Doctor is the preferred varicose vein disease vein specialist in New York and New Jersey. Get back that confidence from veins and pains with the center's multiple minimally invasive and non-invasive treatments for mild and severe varicose veins.
The clinic features the latest in vein and blood vessel treatment technology to treat venous disease problems such as spider veins, chronic venous insufficiency, venous reflux, venous leg ulcers, superficial blood clot, and superficial phlebitis. Call Vein Center Doctor now and ease your varicose vein worries away.