When to Worry About Varicose Veins
Published 2021-07-05
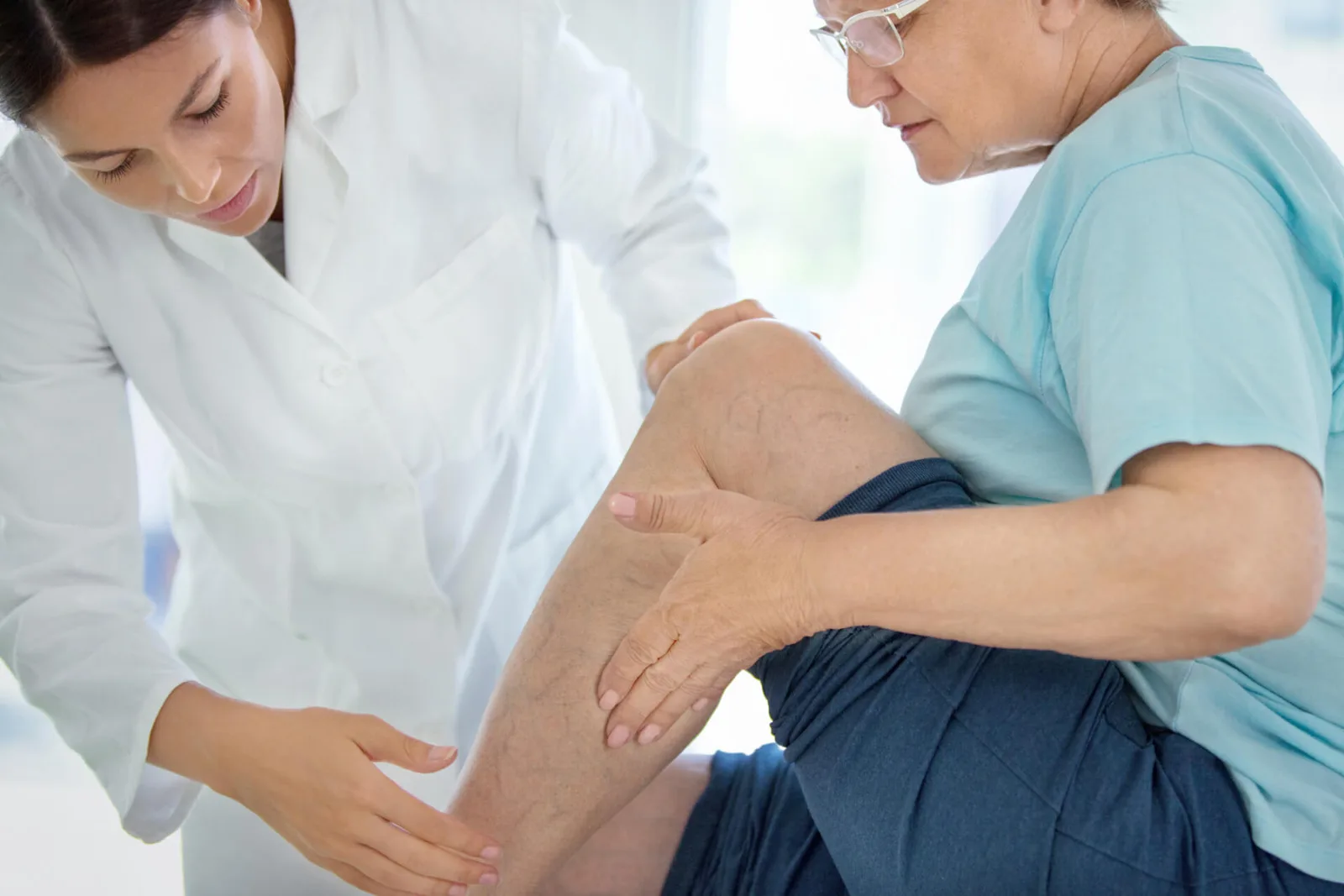
Varicose veins are swelling and bulging veins that commonly develop on the lower legs. A patient may have observed that varicose veins frequently appear - based on the Society for Vascular Surgery, and over one-third of adults in the United States have them. However, most people believe that these bulging veins are merely a cosmetic issue or that there's nothing anyone can do about them.
So when should varicose veins be taken seriously? Untreated varicose veins can develop into a severe vein problem. Although there is no cure for varicose veins, different treatments are available to help lessen the appearance of these visible veins and lower the risk of consequences from these spider veins.
What Causes Varicose Veins?
A weak vein wall and valves are the most common causes of varicose veins. There are small one-way valves inside the veins that open to allow blood flow and then seal to prevent the reverse flow. The blood vessel might get stretched and lose its suppleness over time, resulting in weak valves.
Blood may leak and flow in reverse if the valves do not properly function. If this occurs, a blood clot builds up in the veins causing them to swell and expand -- also named deep vein thrombosis. The reasons for an enlarged vein and the deterioration of vein valves aren't known completely. Some people get the illness for no explicable reason.
A variety of factors can cause varicose veins, such as the following:
- having a blood relative with varicose veins
- being a female
- aging
- activities that involve standing for long hours
- pregnancy
- some underlying vein disease and other conditions
Valves can stop working correctly over time due to corrosion, and the walls of the veins can be less flexible. Blood can reflux and build in the veins of the lower legs as a result of these adverse effects. Chronic venous insufficiency (CVI) is what doctors call it. Blood builds up inside the veins, causing them to swell and twist, resulting in varicose veins.
Moreover, a blocked artery in the lungs causes pulmonary embolism. A blood clot that forms in a deeper vein in the leg and pumps it to the lungs, where it becomes trapped in a smaller lung vein, is the most common cause of such a blockage. Almost all blood clots cause pulmonary embolism developed in the deep leg veins.
When Is Worrying on These Varicose Veins Justified?
Some people observe varicose veins but don't experience any symptoms -- these are called asymptomatic varicose veins. They do not need varicose vein treatment if they are asymptomatic. That means there is no pain involved, swelling, soreness, skin changes, or infections.
However, the evidence implies that they will deteriorate with time and may become symptomatic over time. On the other hand, vein specialists do not believe that treating asymptomatic varicose veins is necessary for medical reasons or to stop the progression. A patient may want to have a superficial vein removed for cosmetic reasons.
Many people are still concerned once they begin to experience symptoms. Ache, swelling, pain along the twisted veins and skin changes, or blood clots are common signs -- known as phlebitis. The first indications and symptoms are usually pain, swelling, tenderness, or pulsation.
Patients frequently report heaviness and fatigue on their legs. That is because blood is accumulating in the leg vein. Skin abnormalities, such as ankle discoloration or stasis dermatitis, are more advanced complications. Blood clots in the veins, also known as phlebitis, are another venous disease.
Moreover, skin disorders might develop, such as ankle discoloration, in which the skin gets red, inflamed, dark, and itching. The bleeding from an affected vein or wounds that do not heal is the ultimate stage. It is known as venous ulcers, and it develops when the skin of the foot and ankle is punctured to the point that it cannot recover.
Every indication should be taken seriously and discussed at a consultation with a vein specialist. The majority are gradual and treated on an opt-in basis. However, if patients notice new signs of swelling, redness, leg pain, bleeding, chest pain, or leg ulcer, immediate medical help is the best option.
The best part is that many treatments are available to help alleviate symptoms and enhance overall vein health. Almost everything can be done in a vein clinic in short operations with less or no disruption. When patients follow their insurance company's healthcare policies, these procedures are frequently covered.
If the abnormal vein becomes bothersome, schedule an appointment to understand more about the treatments available.
Treatment Options for Varicose Veins
Fortunately, therapy seldom requires a stay in the hospital or a lengthy, inconvenient recovery. Varicose veins can usually be treated as an outpatient surgery thanks to less invasive techniques.
Compression stockings. Before continuing to additional therapies, many people start by wearing compression stockings all day. They apply consistent pressure on the legs, assisting veins and leg muscles in circulating blood efficiently. Compression varies depending on the types and brands.
Self-care. Exercise, weight loss, avoiding tight clothing, elevating the legs, and minimizing lengthy periods of sitting or standing are all ways to relieve pain and prevent moderate varicose veins from worsening.
If self-care and compression stockings don't work, or if severe varicose veins are present, a vascular surgeon may recommend one of the following:
Sclerotherapy. In this treatment, a vein doctor will insert the foamy solution into tiny and medium-sized veins, scarring and closing them. Treated varicose veins would diminish in a few weeks.
Endovenous ablation (radiofrequency ablation) cauterizes (burns) and closes varicose veins using radiofrequency waves. Vein doctors perform this procedure to alleviate symptoms such as pain, edema, and discomfort. Ablation is a safe, less invasive procedure than surgery and leaves little or no scars.
Read more: What Are the Options for Varicose Vein Surgery?
Prevention Tips on Varicose Veins
Varicose veins occur whether being a woman, were born into a family with varicose veins, or just getting older.
However, there are a few things patients can do to prevent varicose veins from being more visible, bloated, and deformed, including:
- Avoid sitting or standing in the same position for long periods. Take breaks from the office job to get up and walk around, or get out and stretch legs when traveling long distances. Stretch and exercise the legs as much as possible if working in a "standing" vocation like teaching or retail sales to improve blood circulation and prevent pressure. Wear compression stockings if at all possible, as detailed below.
- Elevate the legs when resting
- Walk regularly as a form of exercise. Maintaining a healthy lifestyle strengthens and tones the leg muscles, improves blood circulation, and keeps body weight in check.
- Constipation can cause varicose veins. Include high-fiber foods in the diet. Fresh fruits, veggies, and whole grains are all rich sources of fiber.
- Use sunscreen regularly (some facial spider veins are caused by too much sun exposure).
- Wear compression stockings.
Read more: How to Prevent Varicose Veins
Remove Superficial Thrombophlebitis Permanently at Vein Center Doctor
Whether you have spider veins, varicose veins, or other types of vein diseases -- Vein Center Doctor has various treatments available. Our team of medical and aesthetics professionals has extensive experience providing non-surgical treatments to remove severe varicose veins and reduce superficial thrombophlebitis.
See a vein specialist at Vein Center Doctor and learn which varicose vein treatment is best for you. Call us today to arrange an appointment.