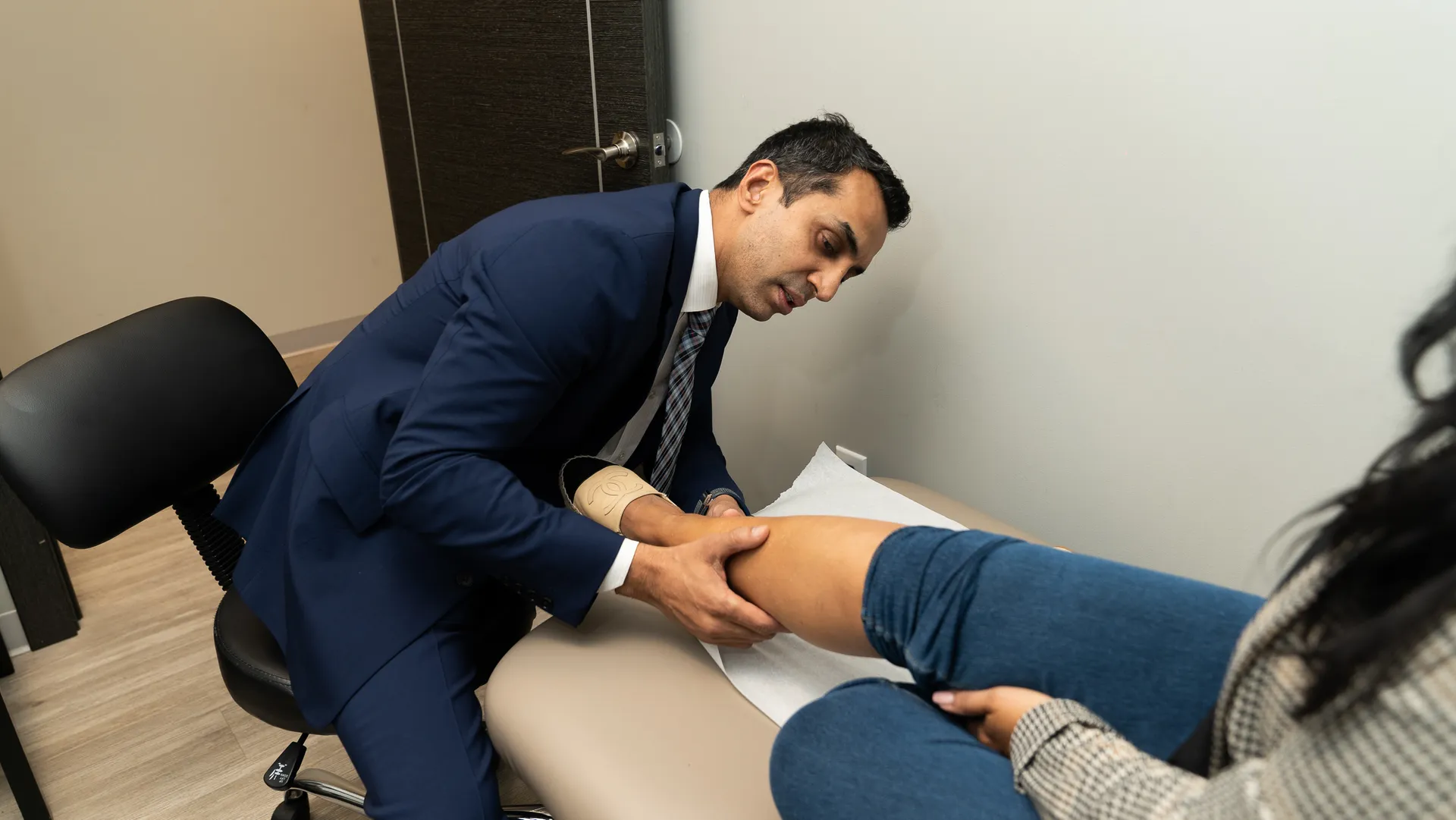
What Your Nurse Does When Assessing Possible Varicose Veins
Published 2023-03-21

Varicose veins are the unsightly appearance of twisted, bulging veins on the legs. While they’re not usually life-threatening, they can also cause discomfort when left untreated. It’s a pretty common problem, so it no longer comes as a surprise when your nurse would also be present when assessing your varicose veins. But some patients ask what nurses are licensed to do for varicose veins.
So what can your nurse do when assessing possible varicose veins? When assessing your legs for varicose veins, a nurse will assist your phlebologist, vascular surgeon, or dermatologist by having you stand for the exam to check the bulging veins more closely. When assessing legs with unilateral edema, nurses should measure the legs and compare their measurements. They can also make a nursing diagnosis of your condition.
How Nurses Assess Varicose Veins
The appearance of varicose veins is a common condition. Because of this, you may find its treatment more accessible with a wealth of solutions. Aside from your doctor, nurses may also be present in assessing varicose veins, where they assist the patient and the practitioner in a more conducive examination. During your assessment for varicose veins, you can expect the following:
1) Physical Examination
The assessment of your varicose veins is performed by a phlebologist, vascular surgeon, or dermatologist, especially when experiencing discomfort from your condition. Nurses may also assist you and your doctor through your examination, keeping your session as conducive as possible.
Your doctor will assess your veins and determine the causes of the appearance of varicose veins to create a treatment plan. A physical examination allows them to gather more information about your condition, reaching an accurate diagnosis. Proper diagnosis is crucial for varicose veins treatment to prevent your venous disease from worsening.
Varicose veins may be caused by different factors which affect your treatment options. These bulging veins may be caused by chronic venous insufficiency or venous stasis, resulting in blood pooling in your legs. They may also be caused by a blood clot in your deep vein or deep vein thrombosis (DVT). During your physical examination, your doctor will start:
a) Interviewing Symptoms
Your doctor will interview you to gather symptoms of your varicose veins and overall health. Varicose veins are usually characterized by the appearance of twisted and enlarged veins at the lower extremity with occasional pain. But they may come with uncomfortable symptoms and even complications, like:
- Heavy or painful sensation in the legs
- Throbbing, burning, or muscle cramping sensation of the legs
- Swelling or edema
- Leg pain that worsens when sitting or standing for a long time
- Itchiness
- Skin discoloration
Varicose veins may also progress into complications, like the development of venous ulcers and blood clots. That's why patients must seek a reputable healthcare provider to receive the proper diagnosis and treatment.
b) Gathering Medical History
Your doctor will also gather your medical history to gauge your risk factors – blood clots in the veins usually recur even after resolution. They will also collect information about your family history and lifestyle to rule out other causes and arrive at a more conclusive assessment of your condition.
c) Observing the Affected Veins
Your doctor will observe your varicose veins closely while standing up. Your nurse will assist the physician and guide you through the process to keep your experience as comfortable as possible. They will have you stand to make the affected veins more visible. This will be difficult to see when you’re lying down, sitting, or having your legs raised. Your doctor might even ask you to describe the aching sensation and leg pain.
2) Diagnostic Test
After your physical examination, your healthcare provider will prescribe an imaging test called venous Doppler ultrasound – this is a noninvasive test that provides an image of the venous blood flowing through your valves. This will give your doctor a more detailed image of your veins, allowing them to detect possible blood clots, faulty vein valves, or other causes of your condition.
Can Nurses Perform Varicose Vein Treatments?
Nurses assist you and your doctor to ensure having a conducive examination for your varicose veins. In some states, nurses can legally perform several varicose and spider veins treatments, specifically sclerotherapy and non-invasive laser treatment. But they must first undergo thorough training for sclerotherapy and laser procedures.
1) How Nurses Train to Help Treat Varicose Veins
Some institutions, clinics, and reputable professionals hold courses on sclerotherapy training for physicians and nurses. Sclerotherapy courses provide hands-on training on how to perform this varicose vein procedure, which might include:
- Venous anatomy
- Pathophysiology of venous conditions
- Complications
- Contraindications
- Patient evaluations
- Injection techniques
- Standards of care
- Information on sclerosing solutions
- Laser solutions
Nurses may also enroll in beauty and aesthetics training involving non-invasive laser treatments on spider veins. Medical professionals seeking to enroll in sclerotherapy and laser procedure courses should seek a reliable institution, receiving lessons from reputable professionals. This ensures having the best practice in varicose vein treatment, not only promoting the safety and satisfaction of patients but also gaining a lucrative skill to your career.
2) Treatments Nurses Can Perform for Varicose Vein Relief
The procedures nurses can provide for treating these venous problems may be limited to sclerotherapy and noninvasive laser treatment. They must first finish the needed training courses and certifications for a license. They may also perform other more elaborate procedures as long as they’re under the supervision of the attending physician
When making a nursing diagnosis for your varicose veins, nurses should also be operating under strict protocol or with the direct supervision of the attending physician. Other diagnoses might constitute unauthorized medical practices.
Recommended Treatment Options for Varicose Veins
Nurses assist you when your doctor assesses your legs for varicose veins. They can also perform some treatments like sclerotherapy and noninvasive laser treatment in some states. But they’d still need to receive training courses to qualify for certification.
Varicose veins are caused by the venous blood collecting in your blood vessels due to having faulty valves – this makes your blood unable to flow back to the heart. The superficial vein starts to get enlarged as the blood pressure increases. Varicose veins may also be a symptom of an underlying condition called deep vein thrombosis. This puts a patient at increased risk of pulmonary embolism.
Varicose veins might be more than just a case of faulty or leaky blood vessels. Patients must seek a phlebologist, vascular surgeon, or dermatologist if there’s a venous ulcer to gain a comprehensive diagnosis and treatment. Some recommended treatments for varicose veins are:
1) Compression Therapy
Wearing compression stockings is one of the most common and effective solutions for preventing and treating varicose veins. Healthcare providers prescribe this whether your condition is caused by chronic venous stasis or a blood clot.
Compression stockings to improve blood flow in the lower extremity. It works by applying pressure to the blood vessels and tissues for pushing venous blood back to the heart. These garments can also relieve leg pain and swelling.
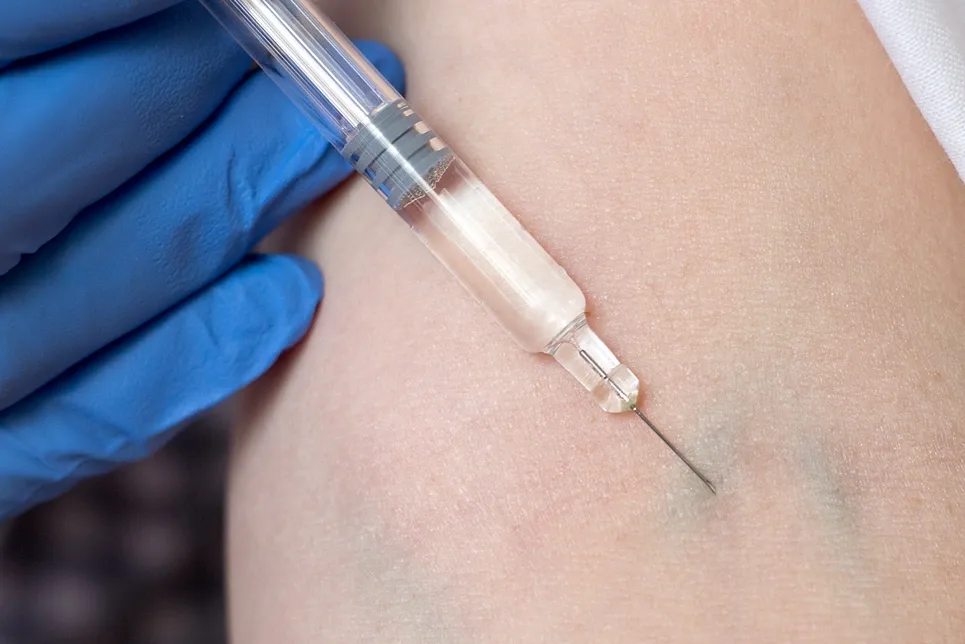
2) Sclerotherapy
Sclerotherapy is also a popular and reliable treatment for removing varicose veins. This minimally invasive treatment involves injecting a solution called a sclerosant into the enlarged and twisted vein. It works by causing a reaction on the venous lining, scarring the vein and eventually closing it up. The treated vein would then be dissolved as local tissues absorb it. The blood would then reroute to other healthier veins.
3) VenaSeal
VenaSeal is a minimally invasive varicose vein treatment involving a medical glue to resolve the enlarged veins. This medical glue will be applied to the affected vein to hold the vein linings together. This procedure will effectively stop the flow of blood in the vein and allow the blood to flow through other healthier veins. Like sclerotherapy, VenaSeal treatment also causes the inactive vein to be absorbed by the body and disappear.
Some varicose veins lie deeper than the superficial vein, making it hard for practitioners to detect them. For these cases, medical professionals like nurses usually use ultrasound imaging to map the affected veins, serving as a guide for the procedure. They will apply the glue by inserting a thin tube or catheter into the vein.
4) Endovenous Ablation Therapy
Endovenous ablation therapy is another procedure for closing off weak or faulty veins to remove varicose veins. This treatment involves applying heat to the lining of the affected vein to damage and close it off.
Endovenous ablation therapy starts with the doctor injecting a needle and wire into the affected vein to insert a catheter. They will then insert specialized tools into the catheter to deliver heat to the vein. The energy will then damage the tissues or lining in the treated vein, closing it. The blood will then flow to other veins. Endovenous ablation may come in different types according to the energy used for applying heat:
- Endovenous laser treatment - uses laser energy to deliver heat.
- Radiofrequency ablation - uses radio waves or radiofrequency energy to deliver heat.
Endovenous laser treatment (EVLT) and radiofrequency ablation (RFA) are both effective options delivering similar results. But in terms of comfort, RFA might be the better option EVLT can be more painful and leave more bruising. This makes RFA the procedure promoting lesser pain during recovery.
5) Ambulatory Phlebectomy
Unlike the prior treatments that close the affected vein, ambulatory phlebectomy offers a different approach to resolving varicose veins. This procedure involves surgically removing the weakened or damaged veins through keyhole incisions.
The vascular surgeon creates small punctures on the skin next to the location of the varicose veins. With a phlebectomy hook, they will bring the affected vein into the surface and pull it out, removing it in small segments. They will use a Doppler ultrasound to detect your veins throughout the procedure. This treatment involves injecting the area with local anesthetics to reduce pain from the incisions and vein removal.
6) Varicose Vein Ligation and Stripping
Similar to ambulatory phlebectomy, varicose vein ligation, and stripping involves removing the affected veins. With this minor surgery, the vascular surgeon will create incisions to reach the weakened vein. They will then tie or ligate the vein by cutting and stitching it. They will then use a wire to remove or strip the vein – this wire will be inserted through the treated vein and brought to the surface, along with the vein, on the other end of the treatment area.
Varicose vein ligation and stripping aim to block blood flow and allow it to reroute to other veins. It’s usually preferred for removing larger varicose veins. Patients taking this treatment option will be under general anesthesia, although other cases are only under local anesthesia. They will be advised to wear compression stockings after the surgery.
Remove Painful Varicose Veins with Vein Center Doctor
Varicose veins are enlarged and twisted veins in the legs, which can cause uncomfortable symptoms like leg pain or skin discoloration. It may also be a symptom of an underlying venous disease. Nurses usually assist patients and doctors during the assessment and treatment of varicose veins. Varicose veins may need a comprehensive treatment plan. They may be caused by leaky valves, deep vein thrombosis, or other conditions.
Vein Center Doctor is one of the vascular centers in New York and New Jersey, offering holistic and integrated treatment plans for varicose veins. With our compassionate and highly-trained medical professionals, patients can expect world-class treatment. We’re also equipped with advanced tools to promote the safest and most comfortable procedures. Get started experiencing relief from varicose veins and book an appointment with us today.