What Happens When a Spider Vein All of a Sudden Has a Huge
Published 2023-06-24
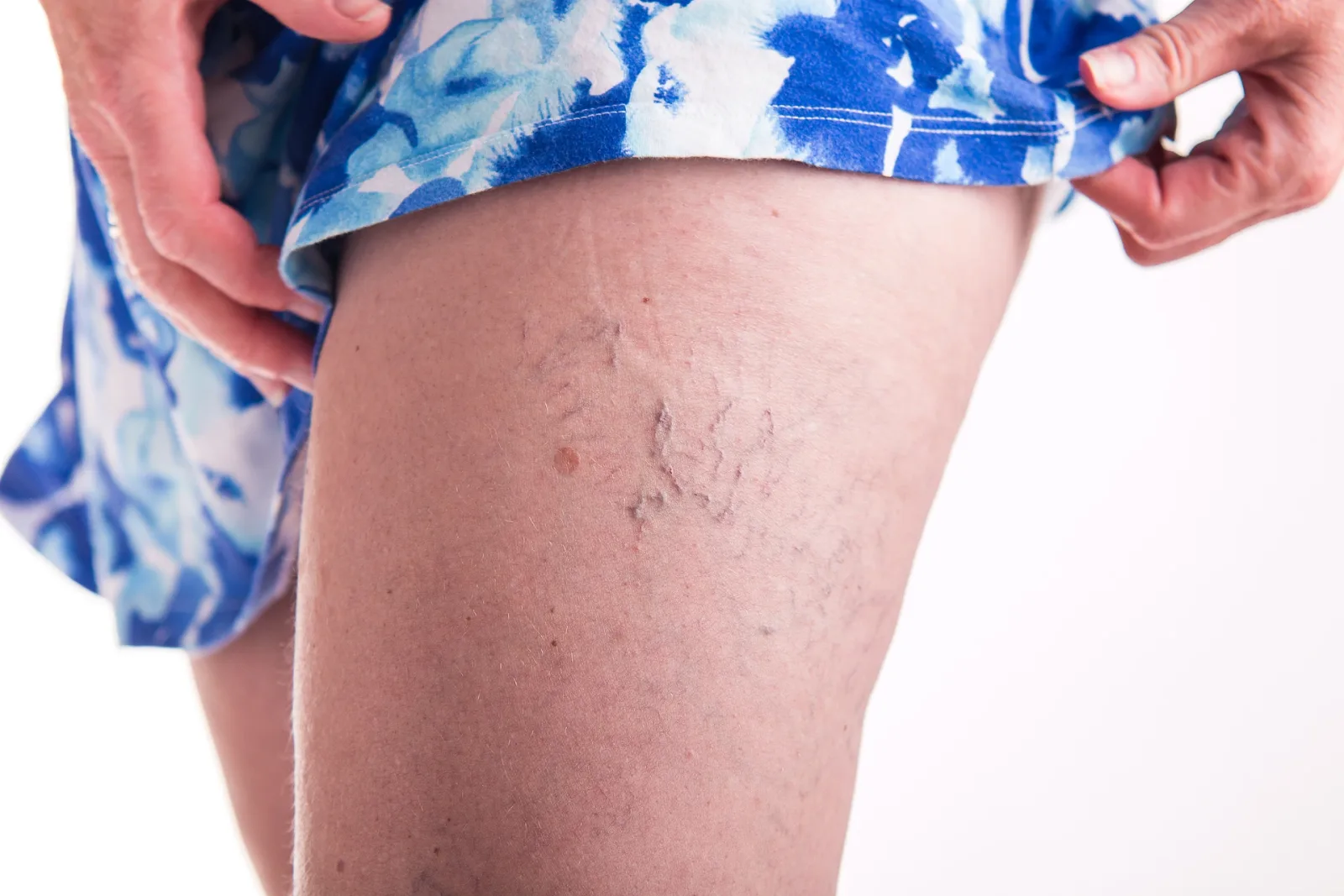
The Causes and Treatment of Enlarging Spider Veins
When a spider vein suddenly develops a large lump that continues growing, it can indicate a dangerous medical issue that requires prompt treatment.
In this article, we’ll take a look at the potential causes — and actions you can take if this happens to you.
What is a Spider Vein?
Those squiggly veins on your legs - called spider veins - are usually just a cosmetic concern. But when one suddenly bulges out in a big lump, it warrants a visit to the doc.
Symptoms of an Enlarging Spider Vein
Signs of an inflating spider vein may include:
- An elevated, knobby, or twisted vein that slowly increases in size over time
- Reddish or discolored skin around the vein
- Irritated, itchy skin
- Tenderness or pain when touched.
This vein enlargement could point to serious problems like venous insufficiency - where the vein walls weaken and blood flow slows - or deep vein thrombosis, a potentially life-threatening blood clot.
If you notice any of these symptoms, see a vein specialist pronto! During your checkup, they'll examine the area and likely recommend tests to rule out worrisome causes. In some cases, treatments like lasers or procedures may be needed.
Risk factors for developing an enlarging spider vein include family history, female hormones, and standing/sitting for long periods putting extra pressure on the veins.
What Happens When a Spider Vein All of a Sudden Has a Huge Lump and Is Growing?
When a tiny vein in your leg suddenly bulges out and expands, it may indicate that a blood clot has formed. These solid chunks of blood can develop anywhere in your body, but they're most common in your legs. If you've got a clot in one of those squiggly surface veins, you should see your doctor straight away.
Unchecked, blood clots can threaten your health in serious ways, like spreading to your lungs - a potentially life-threatening situation called a pulmonary embolism. That happens when part of the clot breaks off, travels to the lung, and blocks a lung artery. Symptoms include sudden shortness of breath, chest pain, and even death in extreme cases.
To rule out a clot, your doctor will need to examine any hard lumps you notice on those twisty surface veins. They'll likely ask about your medical history and give you a physical, possibly ordering an ultrasound scan to confirm the diagnosis. If a clot is present, they may prescribe medicines to dissolve it or recommend surgery to remove it.
Of course, not every firm bump on those squiggly veins is automatically a clot. Sometimes, the bulge could be a harmless varicose vein that's become irritated and inflamed. Still, it's best to get your doc's opinion to rule out anything more serious. Remember: your health is priceless, so seek medical help right away to possibly avoid nasty consequences.
Causes of an Enlarging Spider Vein
Many factors can cause your spider veins to swell up and become more noticeable. Genetics likely plays a role for many people. If your parents or siblings have prominent spider veins, you're more at risk due to possible weak vein walls or dysfunctional valves you inherited.
Some genes linked to enlarging spider veins include:
- COL3A1: Makes collagen for strong vein walls. Mutations cause wall weakness.
- FOXC2: Regulates one-way vein valves. Mutations let blood pool, swelling veins.
Hormone changes affect spider veins, especially in women. Estrogen relaxes vein walls and increases blood flow during puberty, pregnancy, and menopause. This can bulge veins outward.
Certain medical conditions also contribute like blood clotting disorders and venous insufficiency. Some have a genetic basis, increasing spider vein risk.
Genes you inherit and hormones likely account for most spider vein cases. But factors like prolonged standing, obesity, and aging can speed up their widening over time.
While often just a cosmetic annoyance, enlarging spider veins may signal more worrying health issues, so see your doctor for proper diagnosis and treatment. Targeting the root cause - whether genetic predisposition or another medical condition - helps prevent spider veins from worsening.
Poor Circulation
Insufficient blood flow to your veins may cause them to expand and worsen. Your circulatory system must pump oxygen-rich blood to your tissues, so veins can stay healthy. With reduced flow, they can weaken and become twisted or bulging.
Physical inactivity is a major reason behind poor circulation. When you're sedentary for too long, blood supply to your limbs decreases, leading to swelling, numbness and tingling. Certain medical conditions like high blood pressure and diabetes also limit circulation, upping your risk of inflating spider veins.
Other contributing factors:
- Smoking - It damages blood vessels, constricting them and reducing blood flow.
- Stress - It causes vessel narrowing and raises blood pressure, reducing circulation.
- An unhealthy diet - Processed foods and nutritional deficiencies cause clogged arteries, restricting blood flow.
- Some medications - Birth control pills and HRT can imbalance hormones and impair circulation, especially in women. Hormonal shifts during crucial life stages like puberty, pregnancy and menopause already raise the chances of spider veins in females.
Other Medical Conditions or Risks Factors that May Cause an Enlarging Spider Vein
Several health problems and lifestyle factors can contribute to spider veins swelling up.
Cardiovascular issues like high blood pressure, heart disease and kidney disease can impair blood flow.
This increases pressure within your veins, weakening vein walls and making spider veins more likely to balloon outward.
Autoimmune disorders also pose a risk. Lupus and rheumatoid arthritis cause inflammation and damage blood vessels and tissues. This weakens veins and makes them prone to bulging or twisting.
Past trauma to the affected area can set the stage for expanding spider veins. Broken bones or surgeries may disrupt blood flow and increase pressure within veins over time.
Your habits may also play a role:
- Smoking damages blood vessels, reducing flow and stretching veins.
- Living a sedentary lifestyle - with lots of prolonged sitting or standing - raises pressure within your legs' veins, allowing them to distend over time.
Diagnosing the Enlarged Spider Vein
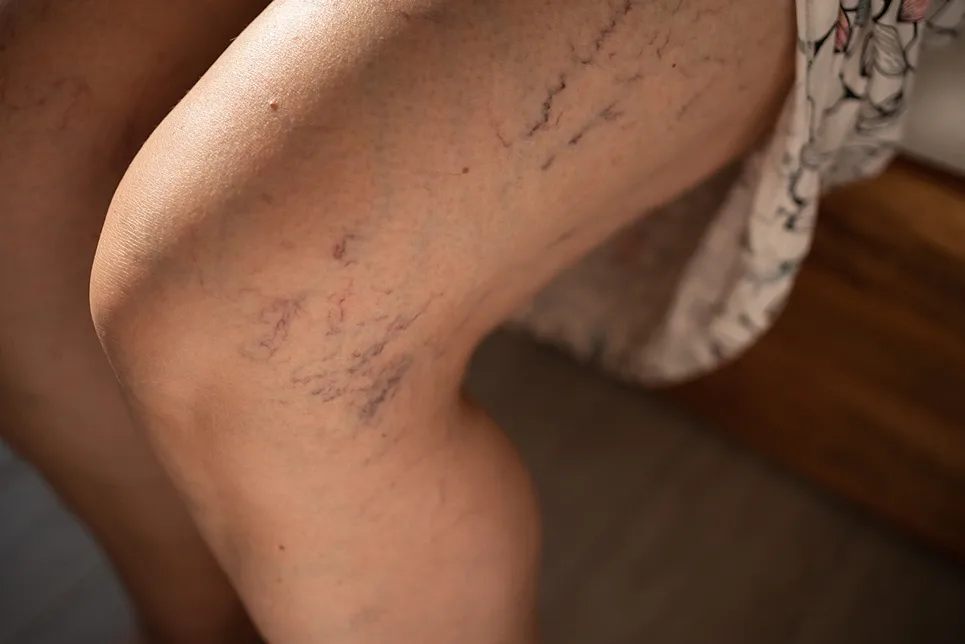
If you notice a spider vein that's expanding, see your healthcare provider as soon as possible. They'll thoroughly assess your condition to determine the cause and best treatment.
During your initial appointment, the focus will be on:
Your Medical History
Your doctor will ask about symptoms, family history of vein issues, hormone changes, and any relevant medications. This helps identify possible contributors like genetics, health conditions, and medications.
A Physical Exam
The doctor will examine the affected vein(s), noting their size, shape, location, and if other visible veins are present. They'll also check your skin for signs of irritation, itchiness and discoloration that signal complications.
This exam helps identify possible underlying health problems that may be causing your spider vein to enlarge, like varicose veins, deep vein thrombosis, and more.
Together, your medical history and physical exam give your doctor important clues to diagnose the main cause of your enlarging spider vein and determine the best treatment approach.
They'll likely consider:
- Lifestyle changes like exercise and weight loss
- Compression stockings
- Medications for certain health conditions
- Cosmetic treatments like sclerotherapy or laser therapy
- In severe cases, surgical removal of the vein
The key is to see your healthcare provider promptly when you notice an enlarging spider vein. An accurate diagnosis and customized treatment plan are the first steps toward keeping your vein issues from worsening over time.
Imaging Tests (Ultrasound)
To diagnose inflating spider veins, vein specialists may use ultrasounds.This noninvasive exam uses high-frequency sound waves that bounce off tissues and create images on screen.
Ultrasounds show how well your vein valves open and close and can spot worrisome blood clots.
Ultrasound-guided foam sclerotherapy is a treatment for expanding spider veins. A solution is injected into the targeted vein under ultrasound guidance, causing it to shrink and reroute blood flow to healthier veins.
Though safe, this procedure can cause bruising, swelling, discomfort, especially:
- You may need compression stockings for up to a week.
- Compression bandages may help reduce swelling.
This treatment works well, easing symptoms of inflating spider veins for many folks.
Treatment Options for an Enlarging Spider Vein
If one of your spider veins starts swelling, several options can help.
Compression stockings are a noninvasive way to shrink inflating spider veins. Custom-fit compression hose gently squeezes your legs, improving blood flow and alleviating symptoms. A doctor or vein specialist can prescribe the right design and pressure for your needs. Proper fit is crucial for comfort and effectiveness, so get measured by an expert.
Sclerotherapy injections involve saline solution injections directly into the affected vein. This seals the vein, rerouting blood to healthier vessels. The quick procedure - lasting under an hour - may require multiple sessions for best results.
Sclerotherapy works well for both spider and varicose vein problems of any severity. Though mildly painful, you can usually return to normal activities right after.
If you notice an expanding spider vein, see your healthcare provider. They'll determine the cause and recommend the best solution:
- Lifestyle changes like exercise and weight loss
- Compression stockings
- Medications for underlying conditions
- Cosmetic treatments like lasers
- Complex vein surgery in severe cases
FAQ: What Happens When a Spider Vein All of a Sudden Has a Huge Lump and Is Growing?
What causes spider veins to suddenly develop lumps?
A lump in a spider vein can indicate a minor blood clot or trapped blood inside the vein, known as superficial thrombophlebitis. This happens when the vein wall becomes damaged or inflamed, causing blood to pool and clot.
Are lumps in spider veins painful?
Yes, lumps or swelling in spider veins can often be painful or tender to the touch. The pain tends to be a dull ache but can also throb or burn. The pain may get worse when standing or walking.
What do I do if I have a painful lump in my spider vein?
You should apply a warm compress to the area, elevate the affected limb, take an over-the-counter anti-inflammatory like ibuprofen, and avoid prolonged standing or walking.
See your doctor if the lump does not start to improve within a week or so, as you may need treatment like sclerotherapy or antibiotics.
Can the lumps in spider veins go away on their own?
Lumps or blood clots in spider veins often go away on their own in 4 to 6 weeks as the body breaks down and absorbs the trapped blood. Keeping the limb elevated, applying warm compresses, and using anti-inflammatories can help speed up this process.
However, see your doctor right away if you notice the lump getting bigger, swelling worsening, or red streaks leading from the area.
Will I need to have my spider veins treated after developing a lump?
It depends on the underlying cause of the lump. If it was due to a minor blood clot that clears up on its own, treatment may not be needed right away. However, the vein damage that led to the clot is still present, so there is a risk of recurrence.
In many cases, the definitive treatment for damaged spider veins that cause clots is sclerotherapy to close off the vein. Your doctor can help determine the best course of treatment based on your symptoms and vein condition.
Conclusion
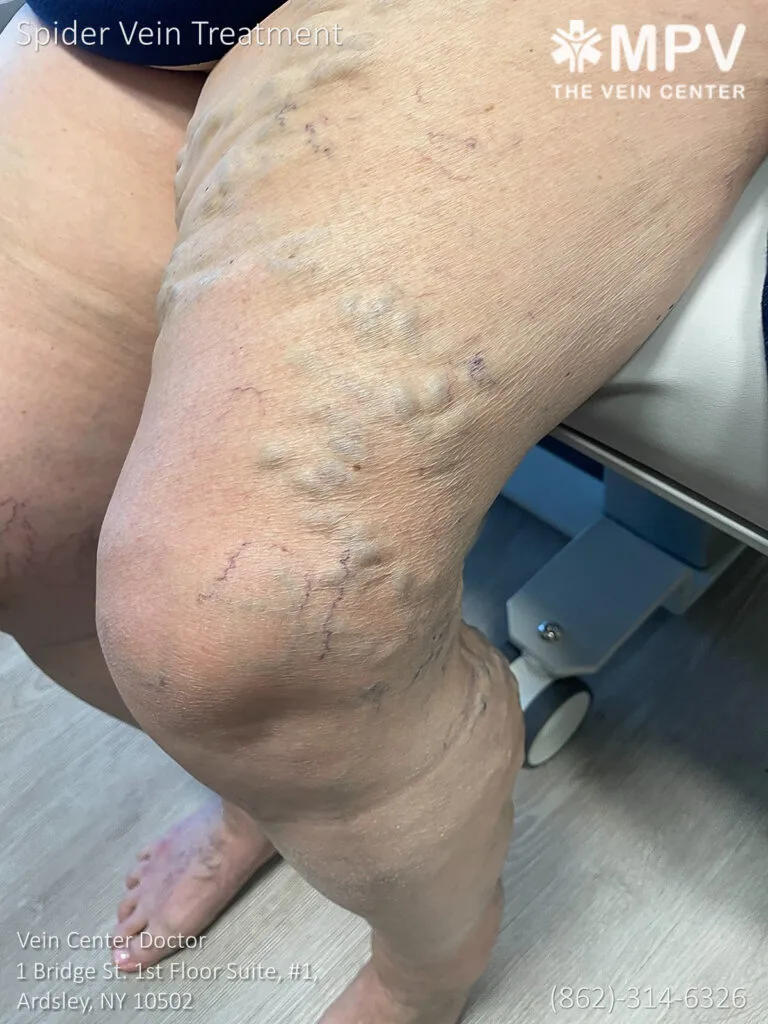
Many options exist for addressing inflating spider veins, from simple compression stockings to minimally invasive injections. Speak with your doctor to find the right path for you. Healthy veins matter! With proper treatment, you'll relieve symptoms and minimize the risk of complications.