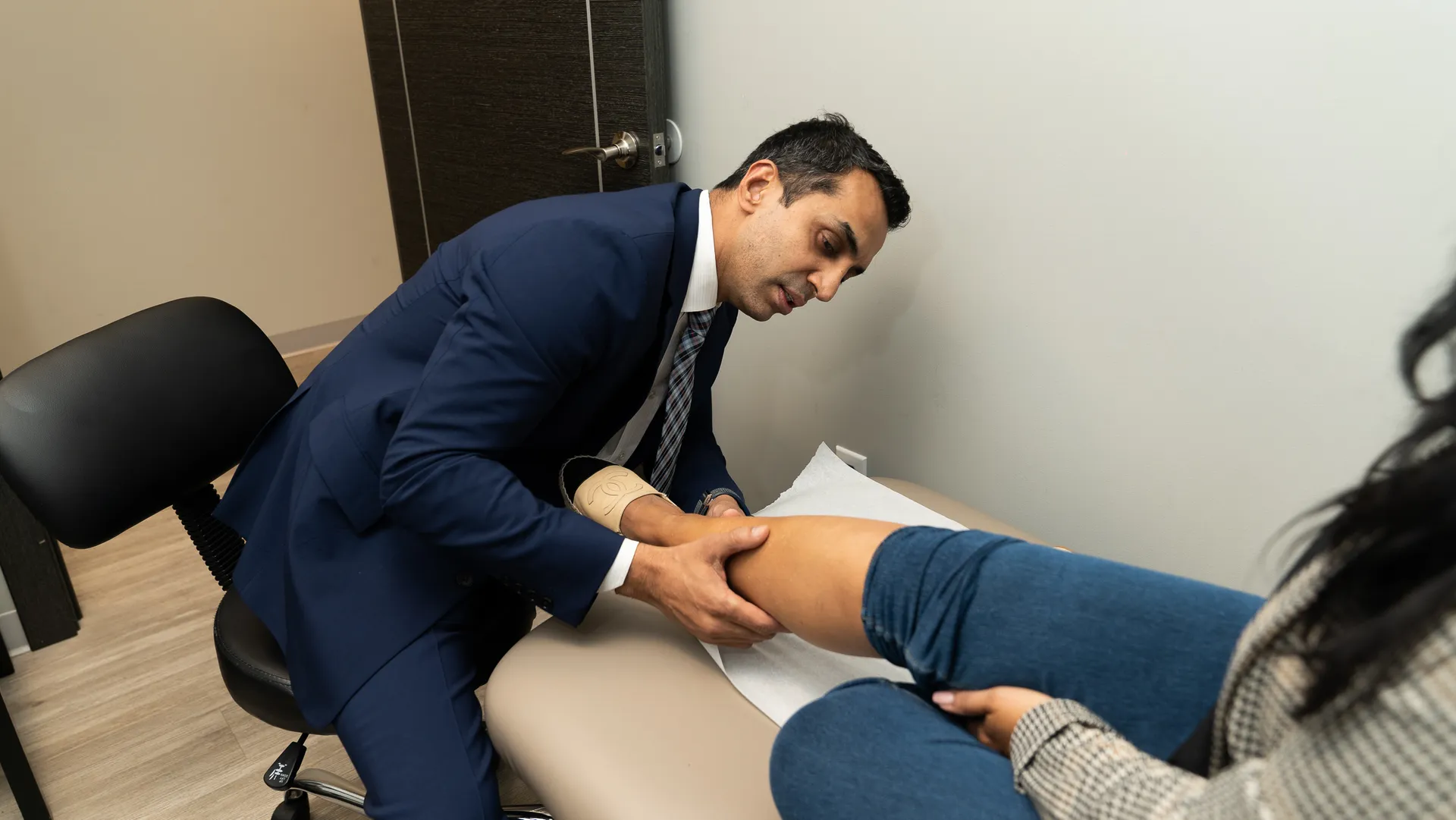
What are the Best Chronic Venous Insufficiency Treatment
Published 2022-10-14
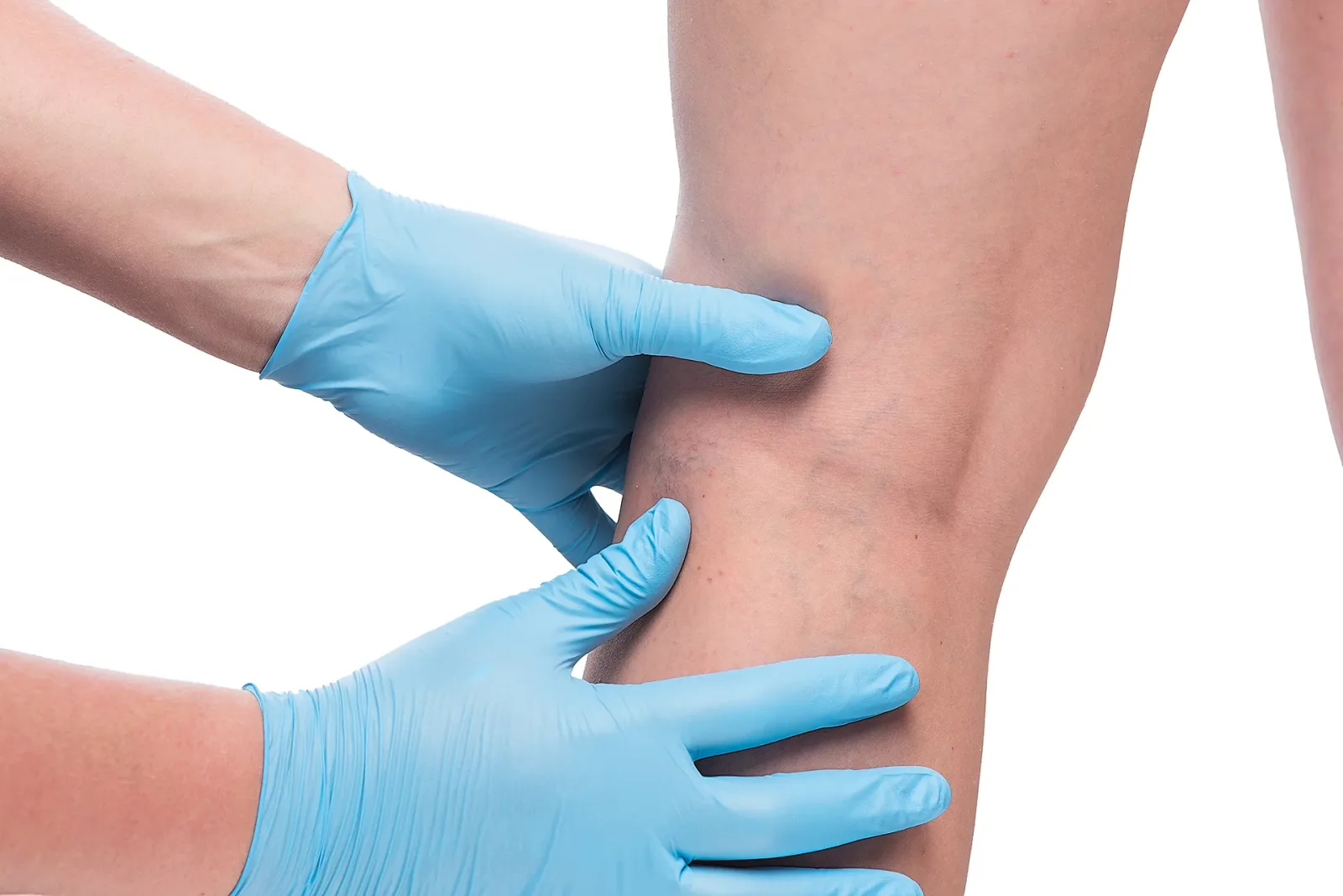
Some lifestyle and genetic factors such as sedentary lifestyle, obesity, smoking, prolonged standing, and lack of exercise can cause poor blood circulation. In the long run, this can lead to varicose veins and chronic venous insufficiency (CVI). Fortunately, a lifestyle change through exercise might also be the key to getting you out of chronic venous insufficiency.
So what are the most recommended chronic venous insufficiency treatment exercise routines? Different low-intensity indoor and outdoor exercises for the lower legs can induce muscle pump function, improving blood flow and alleviating varicose veins and chronic venous disease symptoms. Keep in mind that you should also avoid strenuous activities such as weightlifting can aggravate chronic venous disease, and may lead to worse symptoms such as venous leg ulcer.
Chronic Venous Insufficiency Treatment Exercise Recommendations
Venous insufficiency occurs mostly on the legs, manifesting in most cases as varicose veins and spider veins. Venous pressure from valve incompetence can cause blood to pool in superficial vein systems, resulting in the veins’ protrusion on the skin. This can lead to a limited mobility range and a decreased quality of life in a patient and can progress to symptoms such as lower leg venous ulceration when left untreated.
Muscle pumping function plays an important role in keeping a healthy blood flow from the leg veins to the heart. To be specific, as demonstrated in a 1994 study, calf muscle pumping function is a significant factor in regulating the pneumatic compression pressure responsible for the lower extremities’ venous blood circulation to the heart. For this reason, calf muscles are sometimes referred to as the “second heart” of the body.
This makes leg exercise important for varicose vein recovery, and for reducing venous disease risk factors. To improve blood flow and vein health, reduce varicose vein symptoms and help heal leg ulcers, read on below to find out the best (and the worst) physical exercises for your legs.
Simple Indoor Exercises
The common recommendation for physical activity duration is 30 minutes per day, which you can break throughout the day (e.g., 10 minutes, three times a day). On some days when you might find yourself preoccupied, you can still do some leg exercise to keep your vein health and blood flow at the most optimal.
1) Leg Raises
Leg raises or leg lifts can be done easily without any equipment, or even while working on your laptop. You can either sit upright or lay on your back and lift one leg at a time and hold it for about 5 seconds before slowly putting it down.
The optimal leg lift exercise is recommended to be done for 30 minutes and 3 times a day. When done correctly, leg raises can improve your legs’ blood flow and circulation to the heart, and can ease the leg discomforts you might be experiencing with varicose veins.
2) Calf Raises
The calf muscle pump function mechanism plays a significant role in regulating the venous volume and blood flow, decreasing venous insufficiency and varicose vein severity. As such, to prevent your symptoms from progressing, it might also help to keep those calf muscles moving by making an up and down motion while standing on your tiptoes.
You can also activate your calf muscles through other simple exercises such as rocking your feet back and forth, rolling your feet clockwise and counterclockwise, and lifting your feet upwards. These simple exercises, if done correctly and regularly, can aid in improving varicose vein symptoms and in worse chronic vein disease cases, hasten wound healing in leg ulcers.
3) Lunges
You can also improve your blood flow by activating your leg muscles through lunges. You can begin by standing upright with your legs slightly apart. Then step forward and slowly bend your knee until the knee is directly above your ankle. Slowly straighten your leg as you return to your original position, then do the lunges with your other leg.
Outdoor Exercises
While healing your varicose veins, you might find yourself wanting to step outside for some fresh air at the same time. Here are a few exercises that can help you prevent and alleviate the early stages of chronic venous disease symptoms.
1) Walking
Prolonged sitting and stationary standing are major risk factors for contracting venous disease. Walking, on the other hand, is a low-impact exercise appropriate for improving blood circulation and muscle strength. A brisk walk in your neighborhood or in the park for around 30 minutes each day can prove beneficial in reducing varicose vein discomfort and edema.
2) Cycling
A few minutes of cycling can also do well for your veins. Cycling is a low-impact exercise that does not negatively affect your joints. Cycling action improves your calf muscle strength and calf muscle pump function which aids the venous blood flow in your leg veins to your heart. To maximize its effects, make sure you point your toes to push down the pedal, activating your calf muscles.
Without a bicycle or a stationary bike, you can also replicate this exercise by doing the leg-spinning action at home while lying on your back.
3) Swimming
Swimming is one of the best exercises for improving overall health and is also effective in treating chronic venous disease. Engaging the muscle groups in your legs, arms, and torso through swimming can improve overall blood flow without putting too much strain on your body. The resistance from the water can also aid in muscle toning and blood flow in your leg veins.
Exercises You Should Avoid When You Have Chronic Venous Insufficiency
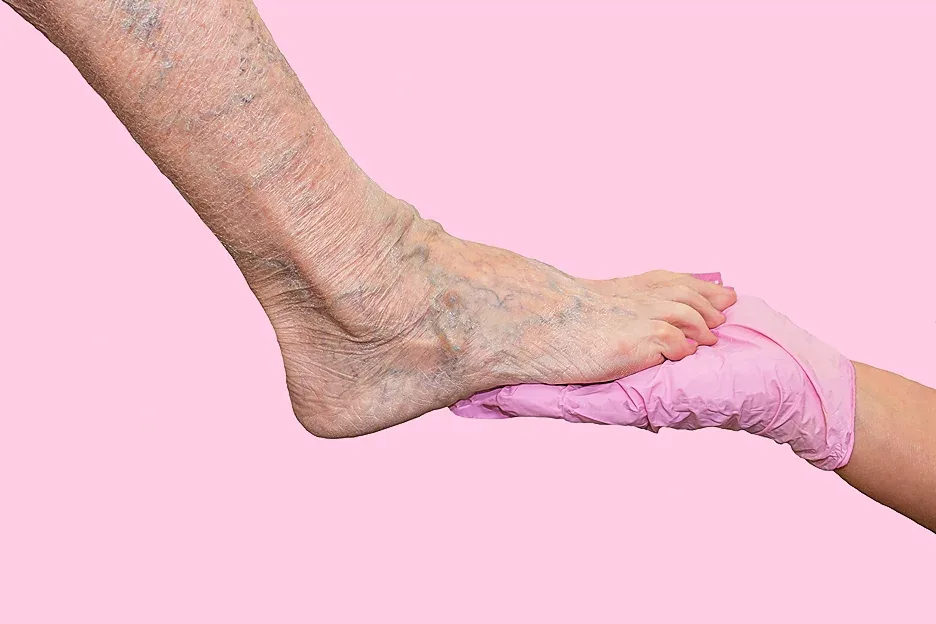
If you have chronic venous insufficiency, it is not recommended to overexert yourself to strenuous activities. Overexerting can lead you to strain your leg veins, causing worse vein disease symptoms such as venous leg ulceration.
1) Weightlifting
Lifting heavy weights is a strenuous activity that increases abdominal pressure, obstructing venous blood flow from your legs to your heart. When this happens, blood accumulates in your legs, increasing venous pressure and worsening venous reflux and varicose vein symptoms.
2) Running
While walking can improve your leg veins’ blood flow, running and jogging are high-impact exercises that can strain your joints and muscles and can even aggravate your veins. High-impact exercises like running can worsen symptoms of chronic venous disease and can lead to venous leg ulcers. When jogging, it can help if you run on softer terrain while wearing compression stockings to soften the impact on your leg veins.
3) Sit-Ups
Another exercise that increases abdominal pressure is sit-ups or crunches. Greater abdominal pressure can also contribute to blood pooling in your leg veins, causing increased venous hypertension and worsening venous disease and varicose vein symptoms.
What Are the Most Common Risk Factors of Chronic Venous Insufficiency?
Chronic venous insufficiency occurs when the veins are unable to efficiently deliver upward blood flow to the heart. Specifically, venous insufficiency is caused by incompetent valves causing venous reflux or backward blood flow. In some cases (i.e., post thrombotic syndrome), it is also caused by deep vein thrombosis (DVT) or excessive blood clot accumulation within the veins, increasing venous hypertension.
When untreated, venous insufficiency can progress to symptoms such as varicose veins and leg venous ulcer. Some of the most common risk factors of chronic venous disease are:
- Prolonged sitting or standing
- Obesity
- Smoking
- Lack of exercise
- Pregnancy
- Heredity
- History of deep vein thrombosis (DVT)
Prevent Severe Vein Complications With Vein Center Doctor’s State-Of-The-Art Vein Treatment Techniques
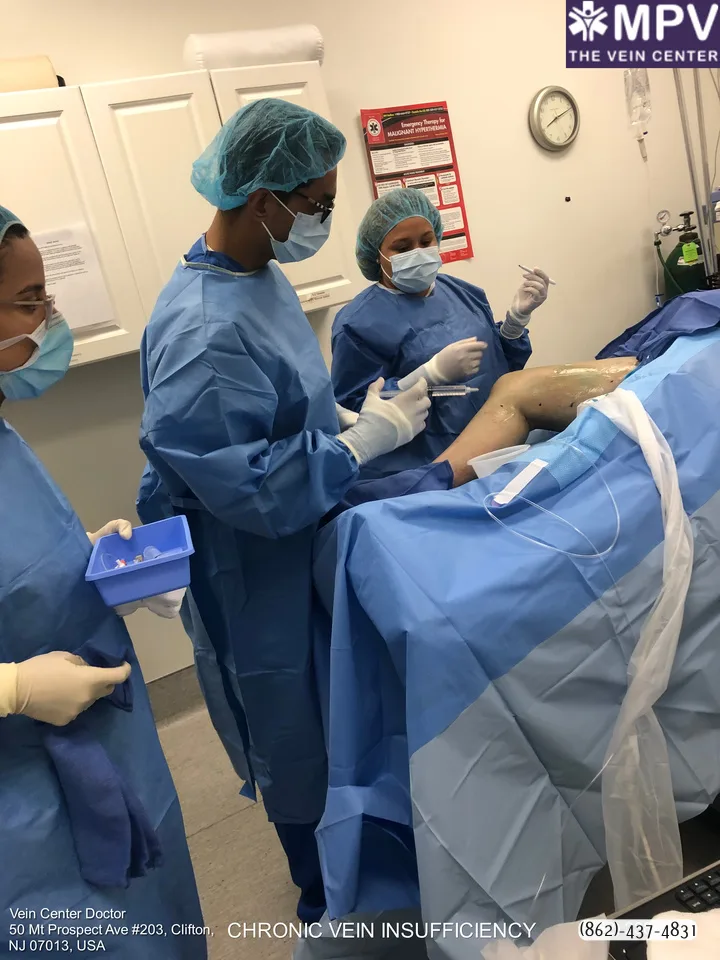
Exercises can help alleviate symptoms, but do not guarantee the patient’s complete treatment. Cases of non-response of chronic venous disease to mild physical exercise are called ambulatory venous hypertension. In these cases, a combination of intervention and compression therapies is recommended.
Here at Vein Center Doctor, our professional vein specialist team offers excellent outpatient vein procedures ranging from compression therapy to laser ablation for varicose veins and chronic venous disease. These procedures are minimally invasive with far fewer risks than vascular surgery procedures such as vein removal and ligation.
Reach out to us now at (862) 500-4747 for your free consultation.