People who have sedentary lifestyles are more likely to develop chronic venous insufficiency (CVI). CVI is one of the most prevalent venous disorders in the United States, affecting as many as 2.5 million Americans each year. To prevent venous disease, more people are looking into physical exercise to encourage proper blood circulation in the body.
But can physical exercise treat symptoms of venous insufficiency? Working out regularly can help ease some of the symptoms but not resolve the underlying vein issues. Pairing your workouts with non-invasive therapies can help your body heal its blood vessels and restore healthy venous function.
Living with unwanted veins is a thing of the past, when you can simply schedule a free consultation with Vein Center Doctor and find your ideal solution today.
Non-ulcerated CVI symptoms are usually felt in the leg. In mild cases, people experiencing venous disease can go about their day without much hassle. But even without a venous leg ulcer, it may still be difficult to perform regular tasks.
Some of the most persistent symptoms include:
This venous disease typically affects the legs, causing pain and swelling near the damaged veins. Pain may get worse after prolonged periods of sitting and standing. Some people may also feel temporary relief after elevating their legs on a stool or stack of pillows. In many cases, the leg pain affects evening sleep and forces the person to repeatedly change positions.
Swelling may also develop in the legs, ankles, and surrounding areas. The swelling usually goes hand in hand with the pain. It also resolves for a while when the leg is placed at an upward angle.
Some problem veins may affect the functioning of nearby nerves. Some pinched nerves may cause numbness in the legs, which can affect a person’s ability to walk. Tingling sensations can also be felt in the lower extremities. While not as pressing as other symptoms, these may affect your ability to focus on daily tasks.
Chronic venous insufficiency is associated with an increased risk of leg cramping. These cramps may happen more frequently at night. Additionally, the cramps may be caused by blood pooling in your leg veins. Cramps that occur even during light activities may signify venous insufficiency.
Practicing regular exercise can ease pressure on the blood vessels and lessen cramping. Drinking 8 to 10 glasses of water a day can also help prevent cramps, as dehydration increases the chance of developing leg cramps.
A structured exercise routine can help ease some symptoms of CVI. Incorporating these into your weekly routines will promote blood circulation in your lower extremities. Some of the most beneficial exercises include:
Walking is one of the easiest exercises since you can practice it anywhere. The movements encourage blood flow in your leg veins, easing some of the venous pressure that causes CVI symptoms. You can start by walking on the way to work, especially if you live near the office.
Some doctors advise against intense running, as the repetitive movement may exacerbate leg inflammation. It’s best to stick to a normal pace of walking to ensure your safety. If you don’t have the time for a light walk during the day, you can also take a quick break every hour and move around your workplace for 5 minutes.
Cycling stimulates blood flow along the leg and calf muscles. At least 30 to 60 minutes of cycling works well for most people. You can practice this routine a few times per week. Cycling also helps people lose weight. Since obesity is a risk factor for CVI, incorporating cycling into your exercise routine may also help you adjust your lifestyle to a healthier one.
Make sure to avoid vigorous pedaling when riding the bike, as intense leg movement may cause cramping. Consult with your doctor to ensure that you don’t exacerbate your symptoms when riding a bike. Some people have advanced venous function problems that can interfere with cycling movements.
Yoga is a popular exercise for people who want to become healthier and lose weight. Many doctors recommend yoga to their patients for its benefits. The movements help improve cardiovascular health and relieve muscular pain.
Some poses can encourage healthy blood flow and ease venous hypertension in malfunctioning superficial veins. These poses raise the feet to an angle above the heart. The following yoga poses may help relieve some symptoms of CVI:
You can either follow yoga guides online or look for a teacher that specializes in healing yoga. Make sure to tell your doctor about your yoga routine to ensure that it’s safe for you. Some people may have other conditions that could be exacerbated by the positions in yoga.
Swimming is a low-impact exercise that helps people lose weight. Besides this, it’s also one of the physical activities that stimulate healthy blood flow in the legs. The water in the pool can also add a healthy amount of venous pressure. Swimming also helps prevent the formation of new varicose veins in the legs.
Just like the other exercises on this list, swimming may not be suitable for all people with CVI. Light strokes are best if you’re not sure of your exercise capacity. If you have an active venous leg ulcer, make sure to wear a water-resistant dressing for safety.
Ensure that you have clearance from your doctor before practicing consistent swimming routines.
Stretching helps ease the venous pressure felt in the legs of patients. One of the easiest exercises you can practice is lunges—these movements target the muscle groups commonly associated with CVI symptoms. Lunges stimulate healthy blood flow in the veins in these areas, preventing more venous valves from malfunctioning.
You can do these by standing and keeping your feet apart. Place one foot forward and bend your knee, keeping it right above the ankle area. Hold this position for a couple of seconds. Return to a neutral position before repeating the movement in the other leg.
Another stretch you can do involves putting your weight on the balls of your feet. Lower your heel and transfer your weight onto it, carefully lifting the ball of your feet. You can do this whether you're standing upright or sitting on a chair. Make sure you have a nearby edge to hold onto for support.
There are some non-invasive forms of treatment that you can use to get rid of your venous disorders. While the effects of exercise on the body are good for your overall health, it’s often not enough to resolve the underlying issues. Exercise is also less effective if you have venous ulceration. A chronic leg ulcer is not likely to heal with conservative treatment alone.
There are 4 different venous treatment plans you can pursue, depending on your desired clinical outcomes. These are sclerotherapy, VenaSeal, venous compression therapy, and radiofrequency ablation.
Sclerotherapy is one of the most common non-invasive treatment methods for CVI. The procedure involves a sealant injected directly into the malfunctioning blood vessel. The operation is relatively painless, thanks to the local anesthesia applied to the area by the doctor.
Specialists directly inject the suspension into the problem vein, effectively sealing it up. The vein eventually collapses before the body reabsorbs it after a few months. Blood originally passing through the vein will redirect into the neighboring blood vessels. Doctors also use sclerotherapy to get rid of varicose and spider veins in the hands, neck, and face.
Slight skin irritation may appear on the treatment site, alongside brown specks and inflammation. These side effects usually go away after a few weeks. Tell your doctor as soon as possible if you still feel discomfort after 7 to 10 days.
VenaSeal is a non-invasive treatment that removes a malfunctioning vein with the help of a special medical adhesive. A catheter is used to transport the sealant inside the blood vessel. VenaSeal is prescribed for patients who have more intense physical symptoms—including persistent inflammation, excruciating pain, and numbed legs. Some cases of varicose and spider veins may also be treated with VenaSeal.
The procedure starts with the application of an anesthetic to the problem veins. A small opening on the skin will be the entry point for the catheter. While the procedure is generally pain-free, patients may feel an uncomfortable sensation when the adhesive enters the vein.
Most patients can resume work, school, and other regular activities within hours after the procedure. Returning to normal physical activity may also decrease the recovery time as it encourages venous function. Take extra precautions not to overexert during the first 14 days, as strenuous physical activities may increase swelling in the treatment location.
Patients may notice visible bruising and redness on the skin after the first few days of treatment. These marks fade over time, although some people may have them for months. A cold compress can help lessen the appearance of bruises. Avoid scratching the area to lessen redness and skin irritation.
CVI patients who have multiple damaged blood vessels may need more than one VenaSeal operation. The time between these sessions depends on the size and severity of the damage in your veins.
Your doctor may also choose to observe how your body reacts to VenaSeal before proceeding with another session. If you experience any harsh reactions even after 14 days, tell your doctor right away.
Venous compression therapy is a non-invasive treatment used to complement other therapies. The compression garments used allow the body to absorb the collapsed veins and redirect circulation to healthier blood vessels. Compression therapy works for nearly all forms of treatment, including sclerotherapy, VenaSeal, and RFA. Some centers also use pumps and other equipment to add venous pressure to the healing area.
The compression garments promote healthier blood circulation in the healthy veins around the removed blood vessel. They make the recovery period faster, although some patients may wear compression stockings for as long as 24 months. Your doctor will base the size and duration of your therapy on the severity of the venous disease.
The garments used to improve your venous disease depend on the size of the vein removed. Some patients may receive prescriptions for tight medical-grade stockings to stimulate venous function.
Compression stockings work best when paired with other venous treatments. On their own, the garments won’t resolve venous reflux. Removing the malfunctioning blood vessel takes care of the problem, while compression garments encourage circulation to proceed in the healthier veins.
Patients may feel slight discomfort in the first few days of therapy. The sensations usually ease after a few weeks.
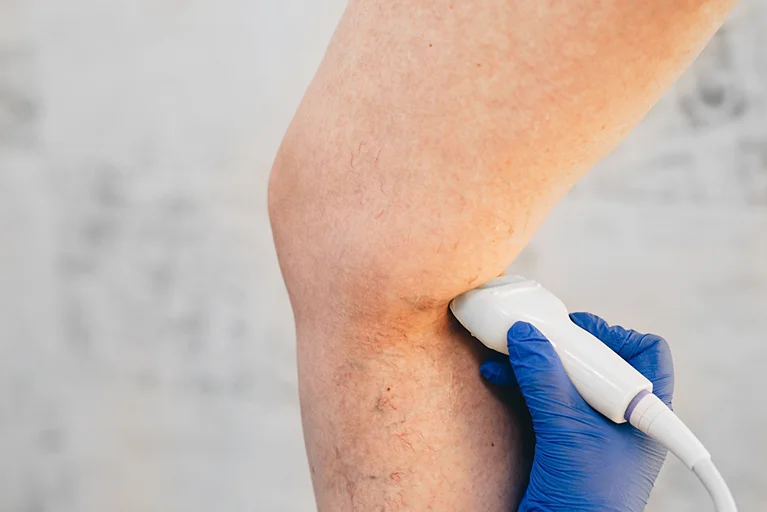
Radiofrequency ablation (RFA) is a form of venous treatment that uses ultrasound waves and an electric current to shut off a malfunctioning vein. RFA is also non-surgical and only requires a tiny incision to allow heat to shut out the vein from blood circulation. Patients can resume their daily activities almost immediately after the operation.
A doctor will use ultrasound to display the direction of the blood vessels in the target area. You will receive a local anesthetic to make the procedure as comfortable as possible. The cut on the skin allows the catheter to directly enter the damaged vein, filling it with heat to seal it shut. Blood flow is diverted into the nearby healthy blood vessels.
You may notice slight bruising and skin discoloration a few days after the procedure. These side effects resolve after a couple of days. Tightness may also be felt in the calf muscles. If you feel any adverse physical symptoms after 2 weeks, contact your doctor right away.
Exercises alone will not treat your chronic venous insufficiency. At Vein Center Doctor, we have a capable roster of specialists that can use non-invasive treatment methods to address your venous reflux and improve your quality of life. We can also help you with any side effects after undergoing your chosen procedure.
We have clinics in Clifton, NJ, and Ardsley, NY. If you have any questions about our treatment offers, you can schedule an initial consultation with our team. You may also reach us at 1-862-500-4747.
Find exactly what you need to get rid of your vein-related problems. Dr. Sood and the rest of our team at Vein Center Doctor are ready to help: schedule your free consultation today.
Most Insurance is accepted for treatment