Is Manual Lymphatic Drainage Effective Against Stage II
Published 2022-09-05

Chronic venous insufficiency (CVI) is often treated with compression therapy and minimally-invasive procedures such as sclerotherapy, vein ablation, ligation, and vein stripping. However, recent studies show evidence of the significant potential of manual lymphatic drainage (MLD) in treating major CVI symptoms, including varicose veins.
So is manual lymphatic drainage an effective treatment for stage II chronic venous insufficiency? MLD aims to primarily treat lymphedema, a condition of tissue swelling due to lymph fluid accumulation through a skin-stretching massage promoting lymph flow. Lymphatics play an integral role in decongesting capillaries and tissues of excess interstitial fluid, thereby alleviating symptoms of chronic venous insufficiency such as varicose veins and chronic edema.
Chronic Venous Insufficiency
Chronic venous insufficiency (also known as chronic venous disease) develops when valves fail to maintain the unidirectional flow of blood from the lower extremity to the heart, leading to complications such as venous reflux, vein dilation, varicose veins, and blood clotting.
CVI mostly occurs in the legs, but its symptoms can also manifest in other parts of the body. When left untreated, CVI can lead to blood pooling in your leg veins, causing venous dysfunctions.
1) Symptoms
The symptoms of chronic venous disease vary according to the type of vein afflicted. However, a patient should be on the lookout for its most common signs and symptoms, which are as follows:
- Persistent pain and numbing sensation in the legs
- Hyperpigmentation, or darkening of the skin in the afflicted area
- Vein dilation, or the appearance of spider veins and varicose veins
- Venous stasis ulcers
- Edema, or swelling in the legs caused by trapped fluid
CVI can be diagnosed by physical examination and medical history-taking, from which it can be determined whether you have a family history of risk factors such as cardiovascular diseases. Ultrasound can also be used as a non-invasive diagnostic procedure for chronic venous insufficiency.
2) Stages
The experienced signs and symptoms of chronic venous insufficiency also depend on the stage at which it’s being diagnosed and treated. According to the clinical classifications from the CEAP convention for the diagnosis of CVI, the stages of chronic venous insufficiency are:
Stage
Severity
Symptoms
C0
mild
No prominent signs of swelling; healthy venous system without blood backflow
C1
mild
Appearance of spider veins/telangiectasia ( < 1 mm) and reticular veins (1 mm to 3 mm)
C2
moderate
Appearance of varicose veins ( > 3 mm); the patient begins to experience swelling and aching of the legs
C3
moderate to severe
Appearance of edema (swelling due to fluid retention in the legs)
C4
severe
Appearance of eczema, skin discoloration, and redness; itchy sensation; flakiness and thickening of skin texture
C5
severe
Open and self-healing ulceration of ankles; increased venous blood pressure due to chronic fluid retention
C6
severe
Severe lower leg ulceration requiring serious wound care
3) Causes
Valvular incompetence can be caused by genetic, environmental, and lifestyle factors that can modify blood pressure, blood flow, and vein tissue integrity. Below are some risk factors that can contribute to primary, secondary, and congenital chronic vein diseases:
- Prolonged standing and sitting
- Obesity
- High blood pressure
- Inactivity and lack of exercise
- Pregnancy
- Deep vein thrombosis (occurrence of a blood clot in deep veins of the legs)
4) Treatments
Thanks to evolving technology, there are various conservative and minimally-invasive treatment procedures suited accordingly for each stage and classification of CVI.
- Compression therapy: This conservative management procedure is the standard treatment for all stages of CVI. It’s commonly administered in conjunction with other surgical treatments.
- Sclerotherapy: In this treatment, sclerosing solutions are administered into the affected vein to block blood pooling and redirect blood to healthy veins. As early as Stage II, sclerotherapy can be administered by the specialist to treat varicose veins.
- Endovenous laser ablation: This procedure use laser fibers inserted through a catheter to destroy the internal vein walls of the affected veins, sealing off the vessel and redirecting blood to unaffected veins
- Vein ligation and stripping: A minor surgical treatment that involves tying the blood vessel affected blood vessel through an incision to seal the blood flow. This is done in conjunction with vein stripping, another surgical treatment that involves full cutting of the affected vein.
- Physical activities: Another simple conservative treatment for chronic venous disease is a structured exercise regimen. Leg elevations are highlighted among exercises that are significantly helpful in improving blood flow and reducing varicose veins.
The Connection Between Lymphatic Dysfunction and Chronic Venous Insufficiency
In 2004, a systematic review by Peter Mortimer and Ian Pearson outlined the effects of chronic venous insufficiency on lymphatic function. This article included the physiology of the normal lymphatic system, the pathophysiology of edema and CVI, and the role of the lymphatic system in maintaining normal fluid homeostasis.
The lymphatic system consists of a network of lymphatic vessels transporting and regulating fluid all over the body, i.e., the lymph. The lymph is a fluid containing bacteria and immune cells such as lymphocytes and macrophages, which are essential for the body’s immune defense system.
The lymphatic vessel network runs in parallel with the cardiovascular system, with its capillaries transporting fluid through intradermal networks. For instance, in the legs, both superficial and deep lymphatic vessels run in association with the saphenous vein and the deep vein respectively, draining to cells in the leg and groin muscles. Like the veins, the large lymphatic vessels also have one-way valves to prevent fluid backflow.
Mortimer and Pearson’s systematic review also highlighted the indispensable role of lymphatic flow in tissue homeostasis. Lymph is produced in most tissues by a net force of blood capillary filtration. Thus, in cases of increased capillary filtration activity and capillary pressure (i.e., venous hypertension), the lymphatic capillary networks are consequently directly affected.
As mentioned, edema is a common symptom of chronic venous insufficiency. Edema refers to the swelling that occurs when lymph fluid accumulates within the leg’s tissues. Edema happens when the lymphatic flow rate is lower than the rate of production of interstitial fluid. This fluid consists of substances filtered by blood capillaries and is supposed to smoothly flow through the lymph vessels and be removed from the tissue.
Thus, edema (or more specifically, lymphoedema) occurs when the lymph drainage is slower than the capillary filtration rate. Capillary filtration, meanwhile, is directly influenced by venous hypertension and high blood pressure which are effects of valvular incompetence and blood aggregation in chronic venous insufficiency.
Accordingly, there is a rich trove of evidence of the concomitant lymphatic pathology associated with blood vessel complications due to CVI. Similarly, congenital abnormality in lymphatic function can also exacerbate edematous symptoms in CVI.
Manual Lymphatic Drainage
Manual lymphatic drainage (MLD) or lymphatic drainage massage is a procedure developed by Dr. Emil Vodder and Estrid Vodder in 1936 to treat swollen lymph nodes. Principally, manual lymph drainage is used to treat lymphedema or the retention of lymph fluid within the tissue.
Lymphedema is also a common side effect after a mastectomy, or breast cancer surgery. Some of its symptoms include:
- Skin discoloration
- Swelling
- Pain
- Thickening of the skin
- Heaviness of the limbs
Lymphedema, like CVI, also has etiological classifications. Primary lymphedema is idiopathic and congenital and results from a spontaneous abnormality in lymphatic development. Whereas, secondary lymphedema is precipitated by a prior injury or associated with lifestyle and environmental factors such as obesity and infections.
1) Procedure
MLD is a skin-stretching massage that aims to promote the movement of lymph fluid through the lymph vessels. It has two phases:
- Clearing phase - releases fluid from the tissues
- Reabsorption phase - directs lymph fluid to the lymph nodes
Lymphatic drainage massage uses 4 main strokes (rotary technique, scoop technique, pump technique, and stationary circles) to stimulate the lymph nodes and promote movement of the lymphatic fluid in the lymph vessels.
Manual lymph drainage therapy is first administered by the lymphedema specialist to unaffected areas to “decongest” and move the fluid away from the affected limb region. Diaphragmatic breathing is advised at the beginning and end of the session to aid in opening deep lymphatic vessels and increasing lymph fluid movement toward the heart.
Lymphatic drainage therapy is usually done by a highly-skilled lymphedema specialist. MLD comes in a variety of techniques, but in brief, these are the common steps:
- Let the patient lie in a supine position
- Encourage deep diaphragmatic breathing at the start and end of the procedure
- Apply gentle pressure
- Apply slow and rhythmical movements
- Treat the unaffected areas of the body first
- Drain affected areas by starting from proximal to distal
Usually, MLD is administered as part of the package of Complete Decongestive Therapy (CDT). This program is a holistic lymphedema treatment that combines MLD with treatments such as compressive therapy, exercises, and skin care.
2) Techniques
There are four techniques used for manual lymph drainage, which are the Vodder, Foldi, Casley-Smith, and Leduc techniques.
- Vodder technique: Uses sweeping motion on the treated area; may also be used for the treatment of fibrosis.
- Foldi technique: Based on the Vodder method, it uses alternating circular strokes and moments of relaxation to treat edema.
- Casley-Smith technique: Uses circular hand motions using the palms and sides of the hands
- Leduc technique: Uses reabsorption movements to collect lymph fluid and direct it to the larger lymphatics
3) Benefits of Manual Lymphatic Drainage
Manual lymph drainage therapy can treat a multitude of health problems aside from lymphedema and other lymphatic system ailments. These include the following:
- Rheumatoid arthritis: The progression of rheumatoid arthritis is often accompanied by poor lymph flow, which leads to further joint pain, tissue swelling, and skin discoloration. To alleviate these symptoms, MLD is used to stimulate lymph flow.
- Fibromyalgia: Fibromyalgia is a condition that causes skin discoloration, tissue swelling, and muscle and joint pain. MLD is proven to be effective in improving quality of life for people affected by this disease.
- Lipedema: In this condition, excess fat that has accumulated in your lower extremity can cause lymphedema by blocking the lymphatic vessels. To prevent further complications, MLD can be used to promote lymph flow.
Is Manual Lymphatic Drainage an Effective Treatment for Chronic Venous Insufficiency?
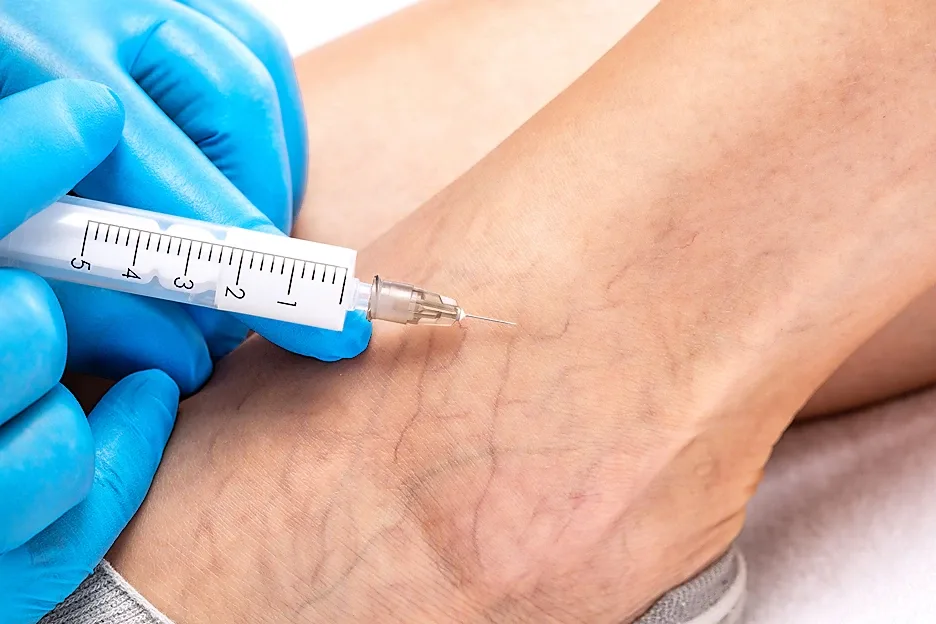
According to a 2013 study, manual lymph drainage therapy has proven effective in increasing venous blood flow in the lower extremity regardless of the presence of CVI. This makes MLD a feasible strategy in the prevention of venous stasis complications in CVI. Consequently, as an effective preventative treatment, it can be as effective in preventing stage II chronic venous insufficiency which manifests itself in varicose veins.
Additionally, a study in 2018 also attested to MLD’s success in improving patient conditions from symptoms regarding ulcer healing and edema alleviation. MLD has also proven effective in reducing limb volume in patients with chronic venous disease, increasing their quality of life. This means that manual lymph drainage therapy can also be used to treat more severe cases of chronic venous insufficiency.
The lymphatic system and the cardiovascular system are parallel networks of fluid exchange. Capillary-level exchanges highlight the interdependence of these two systems, and consequently, this is where the symptoms of resultant cardiovascular and lymphatic disorders originate. Thus, it’s safe to say that a healthy lymphatic system treated by lymphatic drainage therapy can contribute to the prevention of stage II CVI.
Vein Center Doctor: Trusted Healthcare Providers for Your Vein Treatment Needs
Chronic venous disease, if not treated well, can lead to complications that may disturb your quality of life. Non-invasive procedures such as compression therapy and manual lymph drainage must be executed by professional hands with patient-centered attitudes and in-depth expertise.
Here at Vein Center Doctor, our team is always dedicated to providing our patients the vein treatments they deserve. Book a consultation with us now by contacting us at 862-227-1143 (NJ) or (862) 500-4747 (NY) for your free consultation.