Chronic Venous Insufficiency Treatment Guidelines
Published 2022-08-02
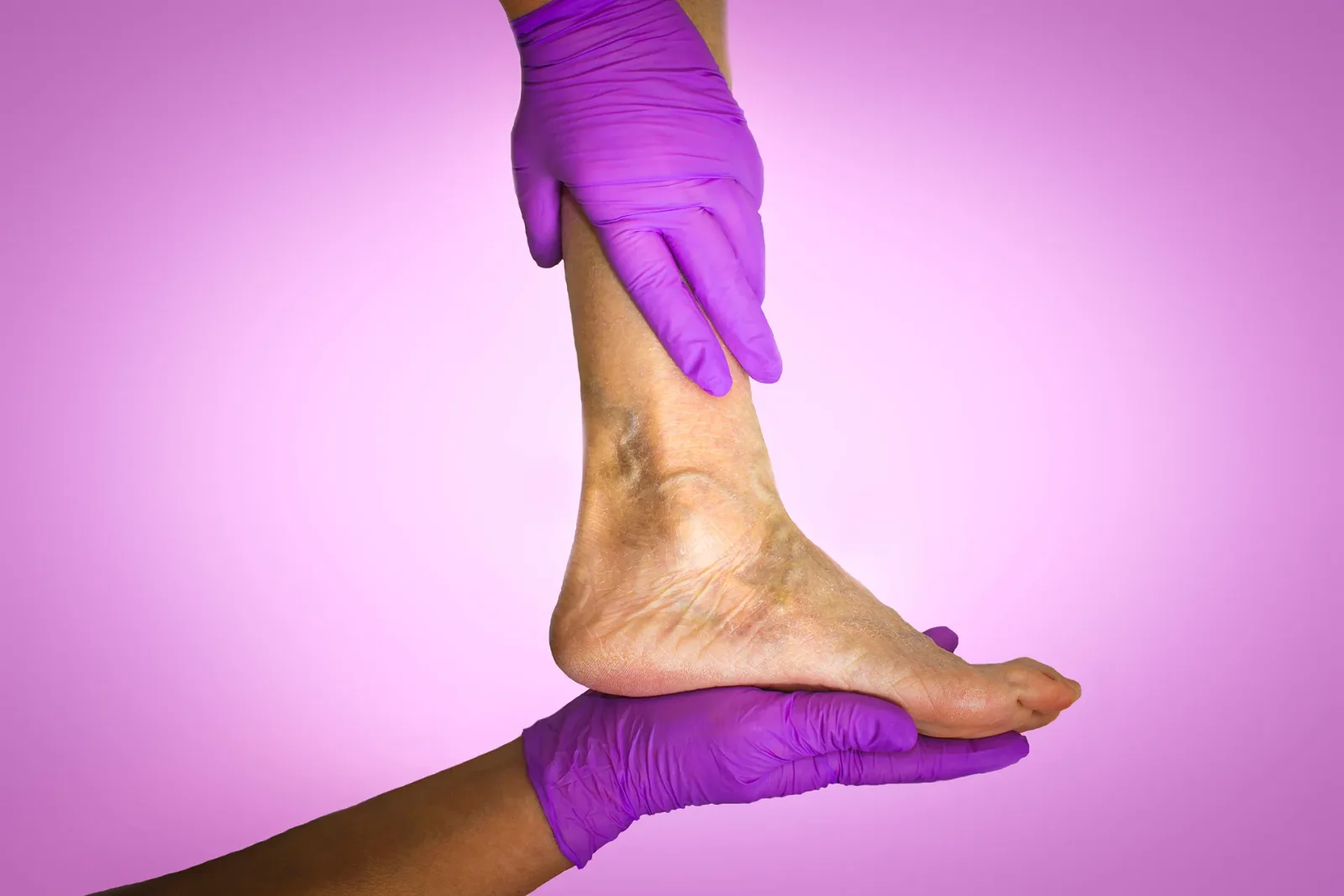
Chronic venous insufficiency (CVI) is a leading venous disease in the United States. Thanks to increased exposure to risk factors, as many as 80% of men and 85% of women are affected by the condition. With long work hours, it’s not surprising that many people have prolonged periods of sitting or standing—increasing the chances of developing venous disorders.
So what can you do to prevent or treat CVI? Regular exercise, diet adjustments, skincare, and adequate rest are excellent starting points to ease your symptoms. Of course, you can also pursue a few noninvasive treatment procedures to eliminate CVI.
Lifestyle Changes to Help Ease CVI Symptoms
The symptoms of CVI or venous reflux may affect your daily functioning. Switching up your lifestyle practices can go a long way in easing your CVI symptoms. Harmful habits, such as a sedentary routine, can contribute to the worsening of your disease.
You can start by slowly incorporating these practices into your daily routine, doing them one step at a time. While these won’t take away your disease, they can also help with the medical management of your venous insufficiency.
Consistent Exercise
Regular physical activities promote healthy venous flow, easing some of the pressure in the veins. Staying active through regular exercise can ease your chronic venous insufficiency symptoms. Some of the most common exercise routines include:
- Walking
- Cycling
- Leg and calf raises
- Swimming
These exercises increase blood flow in the calf muscle, easing some pain and discomfort. They are also associated with preventing ulceration in the body.
Walking is especially helpful since prolonged sitting and standing contribute to chronic venous insufficiency risk. Cycling also encourages healthy blood flow in the calf muscles, especially when you point your toes. This movement strengthens the muscles most commonly associated with malfunctioning vein valves.
Patients with obesity are at increased risk for advanced venous reflux symptoms. Exercises that help burn fat faster include leg lifts, and calf raises. Leg lifts help circulation to the blood, easing pain and swelling caused by venous insufficiency. Likewise, calf raises and light swimming also add a healthy amount of pressure onto the leg veins, which are a common site of CVI.
On the other hand, exercises that involve repeated thrusting of the legs may increase pressure in the veins. These include intense running. Before you incorporate these movements into your daily workouts, consult with your doctor to ensure your safety. You may also pull a muscle if you aren’t careful with your exercises.
Healthy Diet
Alongside regular exercise, eating a healthy diet promotes weight loss and lessens the risk of venous ulcers. A healthy diet is also associated with venous ulcer healing. Additionally, drinking enough water daily can help the body flush out toxins and ease symptoms of venous insufficiency. Adults are advised to drink at least 2 liters per day to promote better health.
A diet rich in fiber also helps healthy weight management.y Women need an average of 25g of fiber per day. Men need a bit more, with 38g as the recommended daily intake. It helps to cut back on red meat, dairy, and sweets to prevent obesity. Varicose veins are worsened by obesity due to added pressure on the veins.
A high-fiber diet also prevents the symptoms of constipation, which can strain the abdominal and leg veins. Some food items rich in fiber include:
- Avocadoes
- Apples and oranges
- Broccoli
- Chia seeds
- Oatmeal
Increasing your potassium intake also prevents cardiovascular disorders, including hypertension and stroke. Food items rich in potassium include bananas, watermelon, potatoes, spinach, and mushrooms.
In addition to fiber and potassium, flavonoids also strengthen your vein walls, lessening the chances of a malfunctioning valve. Flavonoids are substances that act as natural antioxidants. Apples, brussel sprouts, berries, and peaches are good sources of flavonoids.
There are also some food supplements you can incorporate into your diet. Horse chestnut seed extract can help reduce edema and leg pain. French maritime pine bark extract is another source of antioxidants that can help reduce inflammation in the body.
Before taking these supplements, make sure to consult your doctor to avoid any contraindications. Some substances may interact with other medications. The benefits of these supplements are based on a limited trial, so there are no approved therapeutic claims.
Moisturizing the Skin
While skincare may seem like an optional regimen for some people, moisturizing can help prevent the appearance of varicose and spider veins. These veins are often associated with venous insufficiency.
For younger people, exfoliating at night helps encourage proper blood circulation. An antioxidant lotion also promotes collagen production. Additionally, those who like wearing makeup may use variants that include moisturizing ingredients to help protect against varicose veins. Those who have spider veins and bruising may also benefit from using vitamin K cream.
A reliable SPF sunscreen can also help protect against venous insufficiency since sunburns can damage the skin. The resulting cracks may affect your blood vessels, resulting in spider vein formation.
Taking Breaks at Work
Some jobs force people to sit or stand for long periods of time. Without some light movements, at least every hour, blood may pool in the veins. This kind of routine contributes to venous insufficiency symptoms. Taking hourly breaks to walk around helps encourage healthy blood circulation and relieve leg pressure.
It also helps to elevate your muscles. Besides stretching the muscles, elevation also helps prevent blood pooling and venous leg ulcers.
Pharmacological Treatment
Some doctors opt to treat chronic venous insufficiency with drugs. These include aminaftone, a drug mostly used to treat capillary disorders. A controlled trial shows that aminaphtone can help reduce leg cramps, edema, and weakness. Diuretic pills can also be prescribed to lessen leg pressure and improve blood circulation.
Surgical Treatment
There are cases of venous incompetence deemed suitable for surgical treatment. These usually come after all conservative therapies have been exhausted.
The method of surgery depends on the location and severity of the disease. There are three common options:
- Ligation and stripping
- Venous bypass
- Valve reconstruction
Ligation is used in combination with stripping. Vein ligation happens when a doctor makes a small incision and ties the problem veins. In stripping, the vascular surgeon removes a larger problem vein via two small openings in the skin.
Venous bypass is a surgical treatment used for CVI affecting the upper thigh and pelvis. This method is only used in the worst-case scenario since it can be invasive. The procedure works by transplanting a vein from other parts of the body into the affected area, rerouting the blood flow from the damaged vein.
Valve reconstruction is a surgical operation that involves opening the damaged vein. Some vascular surgeons use a procedure similar to a bypass, where damaged venous valves are replaced with those from another person or animal.
The other type of reconstruction uses a small metal stent to prevent the vein from constricting blood flow. This procedure involves a tiny incision in the groin or back of the knee. The vascular surgeon places the stent in the affected vein with help from an X-ray image of the blood vessels.
Best Non-Surgical Treatments Available at Vein Center Doctor
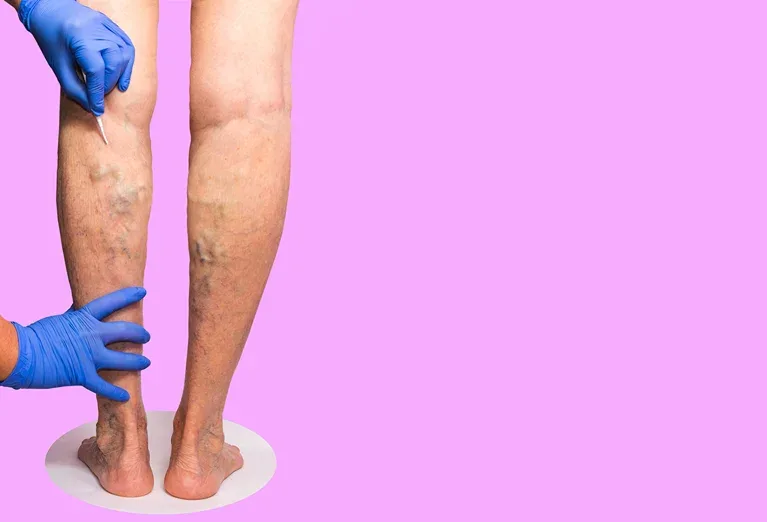
There are non-invasive alternatives to surgery that can also relieve symptoms of CVI and other similar venous diseases. These include the following:
- Sclerotherapy
- VenaSeal
- Venous Compression Therapy
- RFA For Varicose Veins
These treatment methods are available at Vein Center Doctor, a reliable health care provider with extensive experience in handling venous disorders. Unlike conservative therapies, these methods get rid of the faulty superficial veins.
Sclerotherapy
Sclerotherapy is a popular non-invasive alternative to surgery. This procedure is used to seal off problem veins by injecting a solution into the damaged superficial veins. Blood circulation is diverted into the neighboring vessels when the vein walls shut off. Sclerotherapy is also used to minimize facial spider veins. But for most people, sclerotherapy is best to remove valvular incompetence in the legs.
Recovery time from the procedure is generally fast. Some people may develop redness and irritation in the treated area, although this typically resolves after a few days. Patients may also feel slight swelling in the first two weeks.
VenaSeal
VenaSeal involves the use of a special adhesive to seal malfunctioning superficial veins. A specialist applies the adhesive through a catheter inserted into a small incision. The procedure begins when the specialist numbs the area with anesthesia. A small incision serves as the catheter opening. The adhesive travels directly into the vein through the catheter.
Recovery time for VenaSeal is also short. Most patients can resume their usual routines within hours after the procedure. During the recovery period, returning to a normal lifestyle encourages proper venous flow. But to prevent adverse side effects, it’s best to avoid weightlifting and other heavy exercises for at least 14 days.
Patients may develop bruises and patches of discoloration after the procedure. These go away over time, but ice packs can help reduce their appearance.
Venous Compression Therapy
Venous compression therapy is a method used to place a healthy amount of pressure onto freshly treated areas. Compression garments encourage proper venous function in the surrounding area. It’s used for patients who received non-invasive therapies, such as sclerotherapy and VenaSeal.
The dressing is used to pad the treatment site and hasten the recovery process. Additionally, the compression helps lessen venous leg ulcers. Doctors typically ask patients to wear them for at least a few weeks, although the exact time varies per person. The tightness and duration of the compression therapy also depend on the size of the removed blood vessel. It’s good to note that patients may experience a slight itching sensation during their first days of wearing a garment.
RFA for Varicose Veins
Radiofrequency ablation (RFA) is a form of vein treatment that uses ultrasound waves. Doctors distribute electricity into the veins to shut them off. RFA is also non-invasive and has a fast recovery period. Patients can go back to work after a few hours, although intense physical activities should be avoided for the first two weeks.
Doctors use ultrasound waves to create an image of the blood vessels in the symptomatic area. The area is numbed with a local anesthetic. A small incision serves as the opening for the catheter, which is the passageway for the heat from the electric current. The vein eventually collapses and is reabsorbed by the body.
Patients may experience slight bruising in the first 2 weeks. Ice packs can help minimize their visibility. A burning sensation may also be felt at the treatment site.
When to Consider Hospitalization
People with advanced venous insufficiency may develop infections. Besides pain and swelling, fever and pus may also be felt near the location of the affected blood vessel. Some bacteria may not respond well to antibiotics, which can lead to hospitalization.
CVI patients with extremely low or high blood pressure should also receive urgent medical care, as this can lead to other cardiovascular issues. Patients who develop cellulitis and hemorrhage should also see a doctor as soon as possible to prevent extensive tissue damage. Similarly, advanced edema can only be treated with medical pumps.
If you also feel any adverse reactions after a treatment procedure, contact your specialist right away.
What to Do After CVI Treatment
Most venous insufficiency treatment options allow you to resume work right away. The physical activity associated with daily tasks may also improve blood circulation and encourage the body to reabsorb the collapsed veins.
Make sure to avoid consuming unhealthy food, such as those with large amounts of salt and sugar. Drinking enough water (at least 2 liters for adult patients) will also help your body heal faster.
Avoid unnecessarily touching the area to prevent irritation. You should also watch the treatment site every day to prevent bacteria growth. Use only mild soap and lukewarm water to avoid causing more pain in the area.
Have the contact details of your doctor ready. They can help you attend to any side effects after your chosen procedure. Be sure to notify them if you experience any harsh reactions that affect your daily functioning.
Vein Center Doctor: The Best Place to Get Treatment for CVI
People with CVI should have access to top-quality treatment plans. Your disease can worsen if you don’t pursue the right non-invasive venous therapy. At Vein Center Doctor, we have a dedicated team of vascular specialists who can assist you with conditions like deep vein thrombosis, venous reflux syndrome, and other similar disorders.
Our doctors can work with you to create a medical management plan that meets your health and aesthetic goals. For more information, contact us and schedule a consultation at your chosen time.