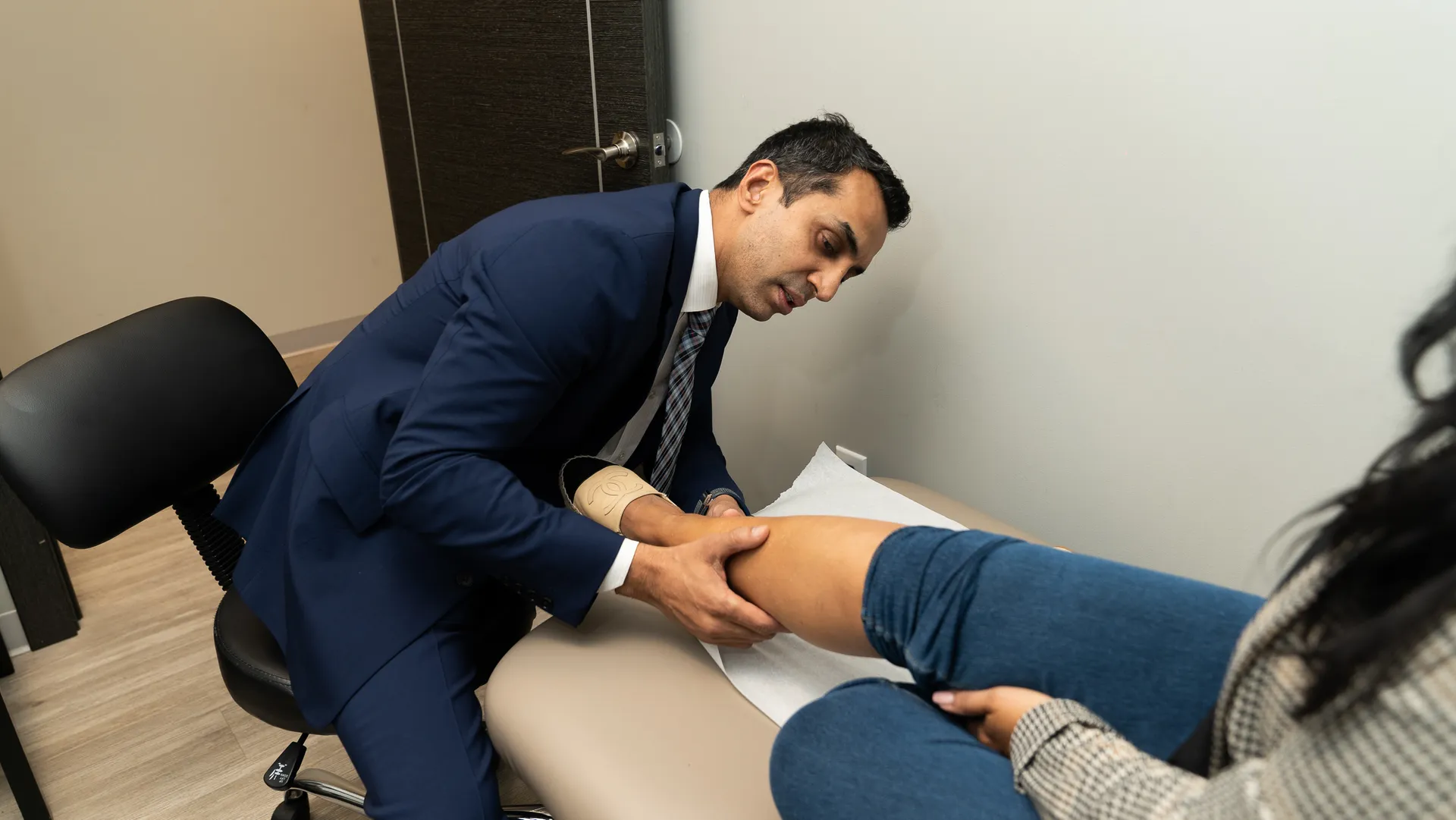
Are Varicose Veins Genetic?
Published 2021-09-20
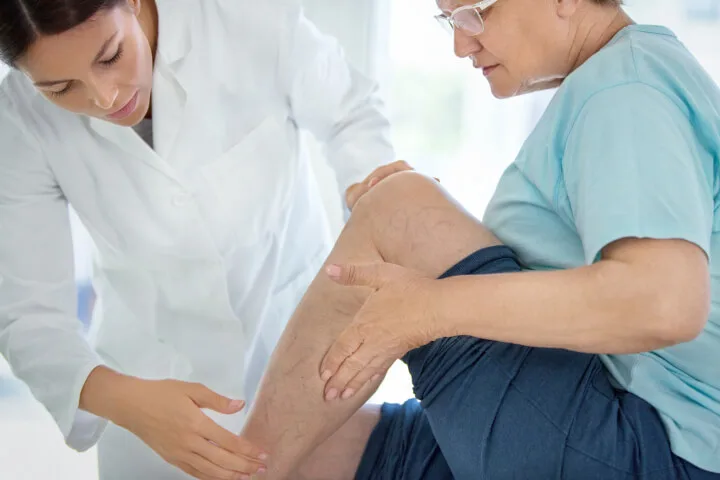
Varicose vein disease is a common issue that affects adults. This vein problem can produce aches, cramps, and throbbing pain in the legs that worsen over time. Either you want to remove them because they’re becoming unsightly or causing leg discomfort, there are many therapies accessible to remove the spider vein and leave behind smooth skin that looks great with shorts or other leg-baring outfits.
So are varicose veins genetic? Experts identified genes that are linked to the pathogenesis of a varicose vein. They showed that venous disease is genetically linked with various traits and phenotypes like the previously identified in an epidemiological study (deep vein thrombosis, venous insufficiency, etc.). They share similar genetic variants with a varicose vein (fluid intelligence, prospective memory scores, and other risk factors).
Genetic Predisposition to Varicose Vein Formation
Varicose vein disease (VVD), the most common type of chronic venous disease, is a multifactorial vein condition. Environmental and genetic factors are both risk factors for developing venous pathology.
A genome wide association study (GWAS) suggests that although heredity is a well-known risk factor for varicose veins, the genetic basis of this vein disease is still poorly understood. The first statement of varicose vein in the PubMed study is from the early nineteenth century.
In the first half of the twentieth century, the study includes the interpretations of the genetic nature of the venous disease. The most judicious of which was provided by a Scientist named Ottley.
Then, after presenting a comprehensive study, the author stated that inheritance happened as per the prevailing form (even the cases of the "missed generation" — the absence of vein disease in one of the generations) of fifty varicose vein treatment cases. It’s due to a higher proportion of patients suffering from vein conditions than with a recessive defect.
In 1949, for instance, American scientists Wagner and Herbut gave conclusions about a genetic factor of a varicose vein based on a histological study. Additionally, they were convinced that dilatation of the vein wall precedes venous insufficiency.
It’s usually functional and secondary, which was later backed by other scientists. In a study of Danish and Swedish scientists Hauge and Gundersen, they highlighted the significance of genetic factors in the etiology of the venous disease.
They concluded that vein disease is implausible to be determined by a single gene based on data gathered from the parents and siblings of 250 patients. In 1974, Czechoslovakian scientists Matousek and Prerovsky projected the heritability of primary varicose veins. It was under the assumption of polygenic inheritance at approximately 50%.
In the West London Study, patients with venous ulcers at their consultations for more than one year had a higher incidence of a venous leg ulcer than a South Asian population. However, the researchers themselves acknowledged a bias in recruitment.
Preceding deep vein thrombosis history, age, vascular disease, and lifestyle (prolonged standing) are primary players in venous ulcers, forming a "cloud" that prevents the identification of possible underlying putative genetic factors. It’s unidentified how many patients with venous reflux in their superficial veins will develop venous ulceration.
In chronic venous insufficiency, iron deposition is associated with the development of skin complications. A functional iron was previously observed, linked gene variants cause lesions in some, but not all, individuals.
A study states that a dysregulated iron cycle causes local iron overload. Also, it can activate matrix metalloproteinases (MMP) and produce free radicals. Moreover, it’s responsible for proteolytic hyperactivity or downregulates MMP tissue inhibitors.
Read More: Varicose Veins and Diabetes: How Are They Related?
Symptoms and Varicose Vein Development
Other than the unsightly appearance, varicose veins may not cause any symptoms. However, if not treated, this venous insufficiency can progress to chronic venous insufficiency (CVI).
This progression may result in an increased risk of symptoms such as:
- Skin color and texture changes
- Skin ulcers that take a long time to heal
- Swelling of the legs, feet, and ankles (edema)
- Leg tingling, burning, and itching
- Severe pain with cramping and aches
- Leg heaviness
Varicose veins are exacerbated by a malfunction in the tiny inner valves that run throughout the veins. These valves manage and direct the blood flow toward the heart. It’s processed from the heart to the lungs, recharged with oxygen before returning to the body via blood vessels.
Once these tiny valves fail to function properly, blood begins to pool, resulting in turn, bulge, and twisted veins. Varicose veins run in families, and hereditary variables are involved in whether or not a patient will develop varicose veins.
Read More: Facial Varicose Veins: What You Need to Know
Other Risk Factors for Varicose Veins
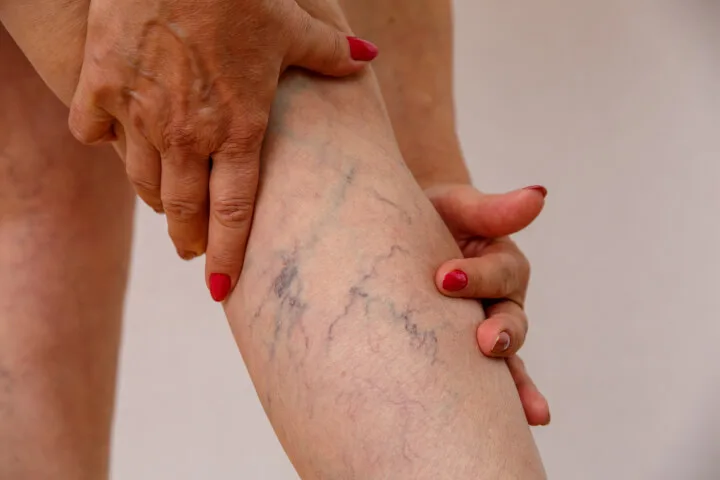
It’s critical to consider that varicose veins are beyond just a cosmetic issue. Many people with varicose veins feel discomfort, throbbing, swelling, itching, or a heaviness in their legs due to their varicose veins.
Learning the causes of varicose veins can help people to understand better the health risks of varicose veins. The following are the major varicose vein risk factors.
Gender — Varicose veins are more ubiquitous in women than in men. Female hormones are considered to be a significant contributor.
Pregnancy — The embryo in the uterus causes pressure on the veins in the lower extremity. It can lead to the pooling of blood in the legs. Fortunately, the varicose veins during pregnancy generally fade after the labor when the increased pressure is relieved.
Weight — Being obese or overweight increases the chances of developing varicose veins. Increased body weight can cause veins to compress, increasing pressure and straining the walls and valves. Weight loss may be beneficial.
Blood clot history — If a patient has had a blood clot or deep vein thrombosis in the past, the chance of having varicose veins increases. It’s due to damaged veins' valves and walls induced by the clot.
Aging — As people get older, veins age as well. Visible varicose veins are more likely to form as the valves and walls cripple over time. That risk rises after the age of 40. It’s critical to remember that aging isn’t the only potential risk for varicose veins.
Damaged veins — If veins are harmed, they may no longer be as strong as they've ever been; they can widen and become varicose veins.
Desk jobs — Jobs requiring sitting or standing all day can put pressure on the legs, leading to the formation of varicose veins.
Experiencing one or more of the given varicose vein risk factors doesn’t guarantee the development of varicose veins. However, a person should consult the doctor when having concerns. Although some risk factors, such as family history and gender, can’t be altered, anyone can make some lifestyle adjustments to help avoid varicose veins from worsening.
Preventive Measures and Effective Varicose Vein Treatment
Even if varicose veins run in the family, there are steps anyone can take to reduce the likelihood of developing them. A few of these simple lifestyle modifications may help reduce or lessen the severity of the symptom.
Exercise the legs. Increasing the activity level by walking and avoiding prolonged sitting or standing can improve blood circulation in the legs specifically, in the saphenous vein where visible veins usually appear.
Lose weight. For overweight or obese, weight loss will reduce the pressure on the veins and may enhance the condition and feel of the legs.
Raise the feet. Elevating the legs above the heart level for 30 minutes, four times daily, can give the veins a break and allow gravity to help the blood flow.
Purchase and wear compression stockings. These distinct stretchy stockings are available at a drugstore, or the doctor may recommend a pair with a particular level of compression. Wear them when getting out of bed in the morning and take them off before bedtime.
Even if some precautions are taken, varicose veins can still develop over time. The good news is that there are more treatment options for varicose veins nowadays than before. Also, remember that surgery isn’t always the best treatment option for varicose veins. Sclerotherapy, endovenous laser therapy, and micro phlebectomy are effective and safe. They’re minimally invasive treatment solutions that a person can consider.
Learn More: What Is a Healthy Diet for Varicose Veins?
Consult With Our Certified Vein Specialist at Vein Center Doctor
Dr. Rahul Sood is the Vein Center Doctor's primary vein specialist. Dr. Sood is a triple board-certified physician and is well known for his extensive cosmetic vein treatments and symptom management assistance. His study and expertise yield excellent results, whether it's treating small spider veins, and another painful varicose vein disease.
Dr. Sood's interest in medical care broadens beyond his work as a vein specialist. He finished his anesthesiology residency at Robert Wood Johnson University Hospital in New Brunswick, New Jersey, and he continues to serve educational communities via lectures and presentations. Book a free consultation with New York and New Jersey's in-demand vein doctor. Contact us today to begin your journey to a healthy vein and skin recovery.