Superficial Vein Thrombosis: When Clots Form Near the Skin
Published 2026-01-15
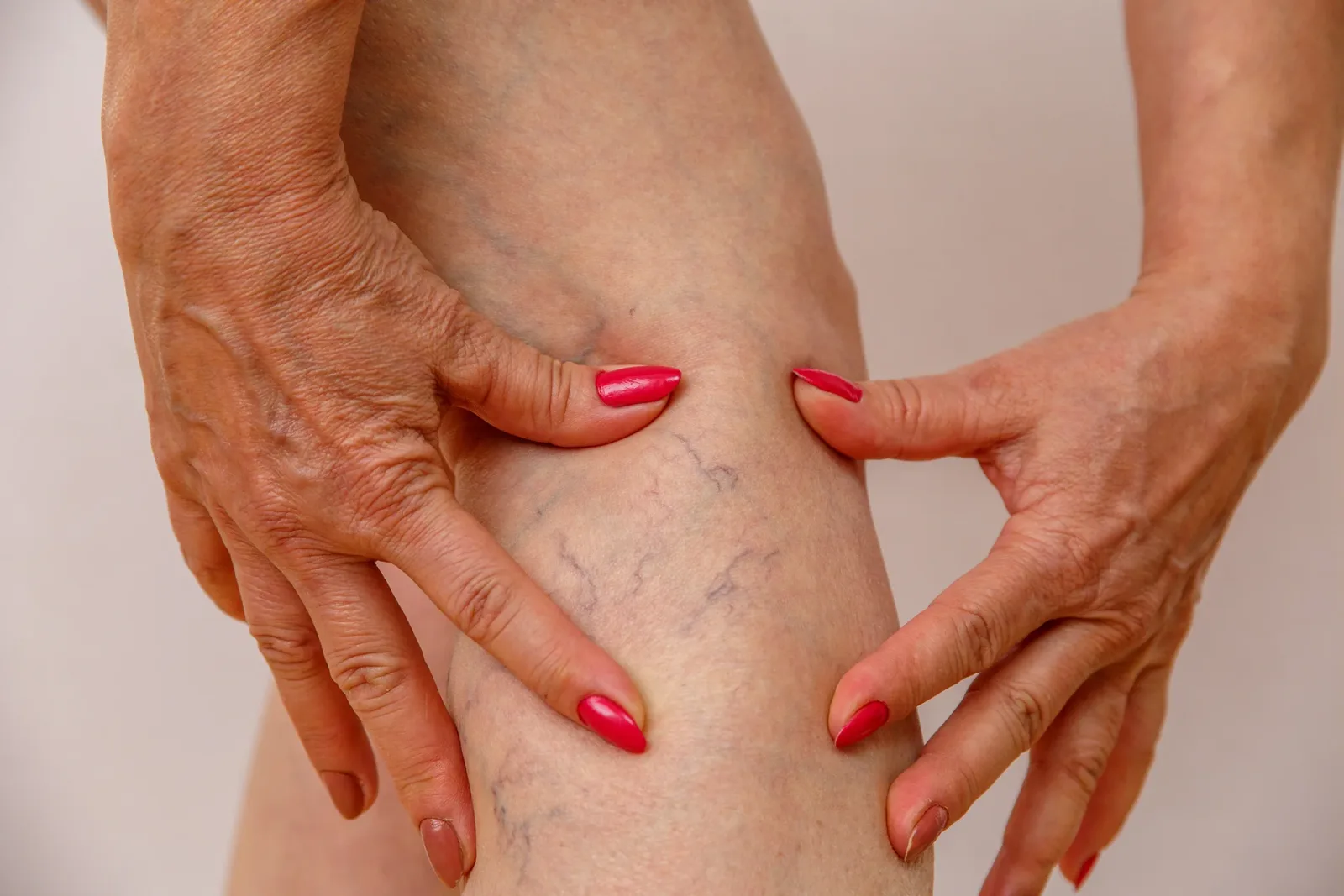
Superficial vein thrombosis (SVT) is a blood clot that forms in a vein just beneath the skin's surface, causing pain, inflammation, and visible skin changes. This condition, also called superficial thrombophlebitis, differs from deep vein thrombosis (DVT) because it occurs in veins outside the deep venous system, though both conditions require medical evaluation.
Superficial vein thrombosis typically affects the legs, particularly the great saphenous vein in 60-80% of cases, but can also occur in the arms, neck, or other areas with superficial veins. While often considered less dangerous than deep vein clots, modern medical research shows SVT carries significant risks and requires proper diagnosis and treatment.
Recognizing the Symptoms: What to Watch For
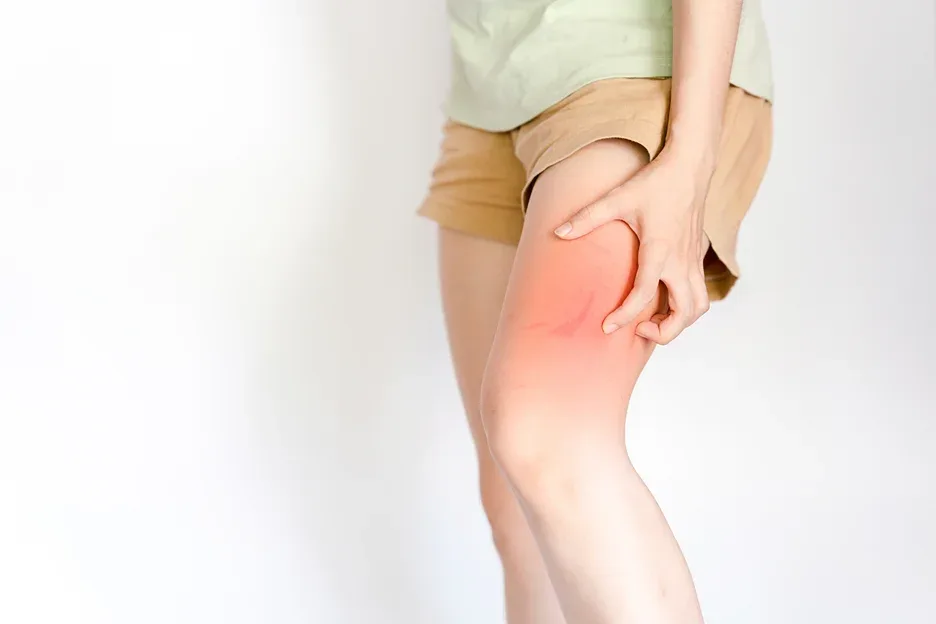
Superficial vein thrombosis presents with distinct symptoms that develop along the course of an affected vein. The most common sign is a painful, tender area that follows a linear pattern just under the skin. This tenderness often accompanies redness, warmth, and swelling in the surrounding tissue.
Patients typically notice a firm, cord-like structure beneath the skin that corresponds to the clotted vein. The skin overlying the thrombosed vein appears red and inflamed, and the area may feel warm to touch. Swelling can occur locally around the clot or more extensively if the condition affects venous return.
In some cases, a palpable lump or knot forms where the clot has created a firm obstruction. The pain usually worsens with pressure or movement and may improve with elevation of the affected limb. Fever can occasionally accompany more extensive superficial thrombophlebitis, particularly if infection is present.
Understanding the Causes and Risk Factors
Blood clot formation in superficial veins occurs when normal blood flow slows or the blood's clotting mechanisms become overactive. Several conditions and behaviors increase the likelihood of developing superficial vein thrombosis.
Varicose veins represent the most significant risk factor, as the dilated, tortuous veins create stagnant blood flow that promotes clot formation. Prolonged immobility, whether from long travel, bed rest, or sedentary work, similarly reduces venous circulation and increases clotting risk.
Hypercoagulable states from genetic conditions substantially elevate SVT risk. These include factor V Leiden mutation, prothrombin 20210A mutation, and deficiencies of protein C, protein S, antithrombin III, or factor XII. Malignancy also increases clotting tendency, making cancer patients more susceptible to superficial thrombosis.
Hormonal factors play a crucial role, with pregnancy, birth control pills, and hormone replacement therapy all increasing clotting risk. Recent surgery, trauma, or intravenous catheter placement can directly damage vein walls and trigger thrombosis. Inflammatory conditions and infections may also precipitate superficial vein clots.
Diagnosis: How Vein Specialists Confirm SVT
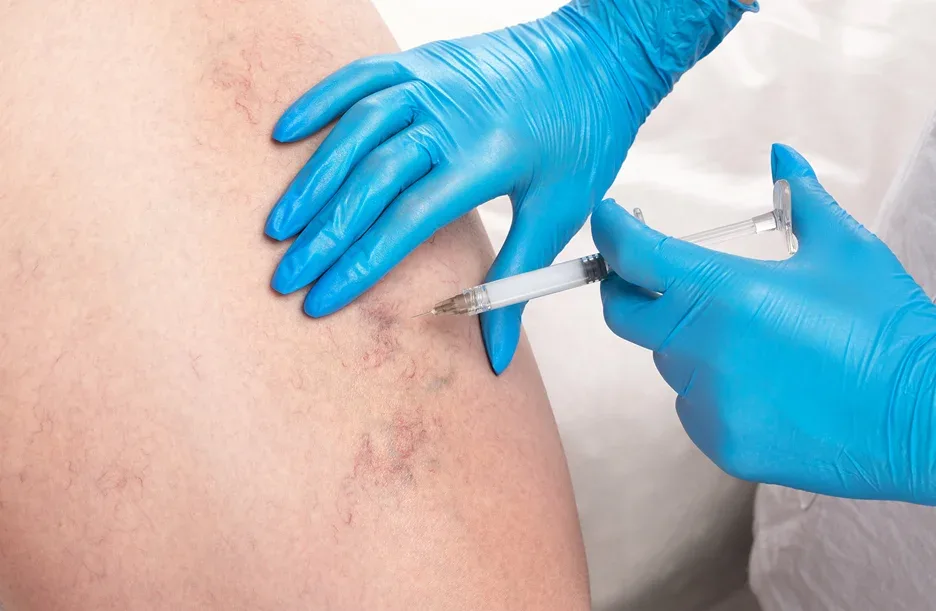
Diagnosis of superficial vein thrombosis begins with a thorough physical examination, as the characteristic signs are often visible and palpable. Vein specialists assess the location, extent, and tenderness of the affected area while evaluating for signs that might suggest extension into the deep venous system.
Duplex ultrasound serves as the primary diagnostic tool, providing detailed images of the superficial veins and confirming the presence, location, and extent of the clot. This non-invasive test also evaluates blood flow patterns and determines whether the thrombosis approaches the junction with deep veins, which significantly changes treatment considerations.
In ambiguous cases or when clinical suspicion remains despite negative initial imaging, repeat ultrasound may be necessary. Blood tests help identify underlying clotting disorders or inflammatory markers, particularly for recurrent or unusual presentations. If infection is suspected, blood cultures guide appropriate antibiotic therapy.
Treatment Options: From Conservative Care to Medical Intervention
Treatment goals for superficial vein thrombosis focus on reducing local inflammation, preventing clot extension, and minimizing the risk of venous thromboembolism. Management strategies range from simple home measures to prescription medications and surgical interventions.
Conservative Management
For mild cases involving short segments of superficial veins, conservative treatment often proves sufficient. Elevation of the affected limb reduces swelling and improves venous return. Compression stockings or bandages provide external support, reduce pain, and limit clot progression.
Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen address both pain and inflammation. Warm compresses applied to the tender area can improve comfort and promote resolution. Regular walking and gentle movement encourage circulation without placing excessive strain on the affected vein.
Medical Therapy
Patients with extensive clot segments (generally 5 cm or longer), thrombosis near deep venous junctions, or significant risk factors require anticoagulation therapy. Fondaparinux, a synthetic anticoagulant, reduces the risk of clot extension and subsequent venous thromboembolism.
Treatment duration typically spans 45 days, balancing the benefits of preventing progression against bleeding risks. For patients with contraindications to anticoagulation or those who fail medical therapy, surgical options may be considered. Blood thinners are also recommended for recurrent SVT or when the condition occurs in unusual locations.
Surgical Interventions
Surgery plays a limited but important role in selected cases. Ligation of the saphenofemoral junction prevents clot extension from the great saphenous vein into the deep femoral vein. Stripping thrombosed superficial veins removes the inflamed segment, providing symptomatic relief.
Local thrombectomy, or clot removal, may be performed for isolated, painful segments. However, surgical approaches carry their own risks of venous thromboembolism, making patient selection critical. Most guidelines reserve surgery for cases with clot extension to within 1 cm of deep venous junctions, anticoagulation failure, or intense pain unresponsive to conservative measures.
Potential Complications: Why SVT Requires Medical Attention

Historically viewed as benign and self-limited, superficial vein thrombosis is now recognized as having significant potential complications. The most serious concern is progression to deep vein thrombosis, occurring in up to 15-20% of untreated cases.
Pulmonary embolism, while less common than with DVT, can occur if a superficial clot extends into deep veins and fragments travel to the lungs. The risk increases substantially when thrombosis involves the proximal saphenous veins near their junctions with deep veins.
Recurrence represents another important complication, with affected patients facing increased risk for future venous thromboembolic events. Chronic venous insufficiency may develop if valve damage occurs within the affected superficial veins, leading to long-term leg swelling, skin changes, and ulcer formation.
Prevention Strategies: Reducing Your Risk
Preventing superficial vein thrombosis involves addressing modifiable risk factors and maintaining healthy venous circulation. Regular exercise, particularly walking, promotes calf muscle pump function and venous return. Avoiding prolonged sitting or standing reduces venous stasis, with movement breaks recommended every hour during long travel or desk work.
Maintaining a healthy weight decreases pressure on leg veins, while smoking cessation improves vascular health and reduces clotting tendency. For individuals with varicose veins, compression stockings provide ongoing support and may reduce SVT recurrence.
Proper hydration prevents blood from becoming overly viscous, particularly during air travel or in hot environments. For high-risk patients, such as those with previous clotting events or genetic predispositions, medical consultation may identify needs for prophylactic measures during high-risk periods like surgery or pregnancy.
When to Seek Immediate Medical Care
Certain situations warrant urgent medical evaluation for suspected superficial vein thrombosis. Rapidly worsening pain, increasing redness, or expanding swelling suggests clot extension and requires immediate assessment. Fever, especially with severe pain, may indicate septic thrombophlebitis, a serious infection requiring antibiotics.
Shortness of breath, chest pain, or coughing up blood could signal pulmonary embolism and demand emergency care. Any superficial thrombosis occurring near the groin (saphenofemoral junction) or behind the knee (saphenopopliteal junction) carries higher risk of deep vein involvement and should be evaluated promptly.
Patients with cancer, previous DVT/PE, or known clotting disorders should seek early medical assessment for any suspected SVT. Similarly, those on anticoagulation therapy who develop new superficial clots need evaluation to ensure treatment effectiveness.
Living with Superficial Vein Thrombosis: Recovery and Follow-up
Most cases of superficial vein thrombosis resolve within 2-6 weeks with appropriate treatment. During recovery, patients should continue compression therapy, maintain regular activity, and follow up with their vein specialist to ensure complete resolution.
Repeat ultrasound may be recommended to confirm clot resolution and exclude extension into deep veins. For patients with recurrent SVT, investigation for underlying clotting disorders or malignancy may be appropriate. Long-term management focuses on preventing recurrence through risk factor modification and, in some cases, extended anticoagulation.
Understanding superficial vein thrombosis empowers patients to recognize symptoms early, seek appropriate care, and prevent complications. While often less severe than deep vein thrombosis, SVT requires medical evaluation and treatment to ensure optimal outcomes and minimize the risk of progression to more serious venous thromboembolic events.